Introduction:
Shingles, caused by the reactivation of the varicella-zoster virus, presents a unique set of symptoms that can often be mistaken for other conditions, including insect bites. This confusion can lead to misdiagnosis and inappropriate treatments. Understanding the visual characteristics of shingles, distinguishing it from bug bites, and recognizing the importance of accurate diagnosis are essential for effective management. This article delves into the nuances of shingles and its symptoms, providing clarity on how it can resemble insect bites and what steps should be taken when encountering such a rash.
Understanding Shingles: Symptoms and Visual Characteristics
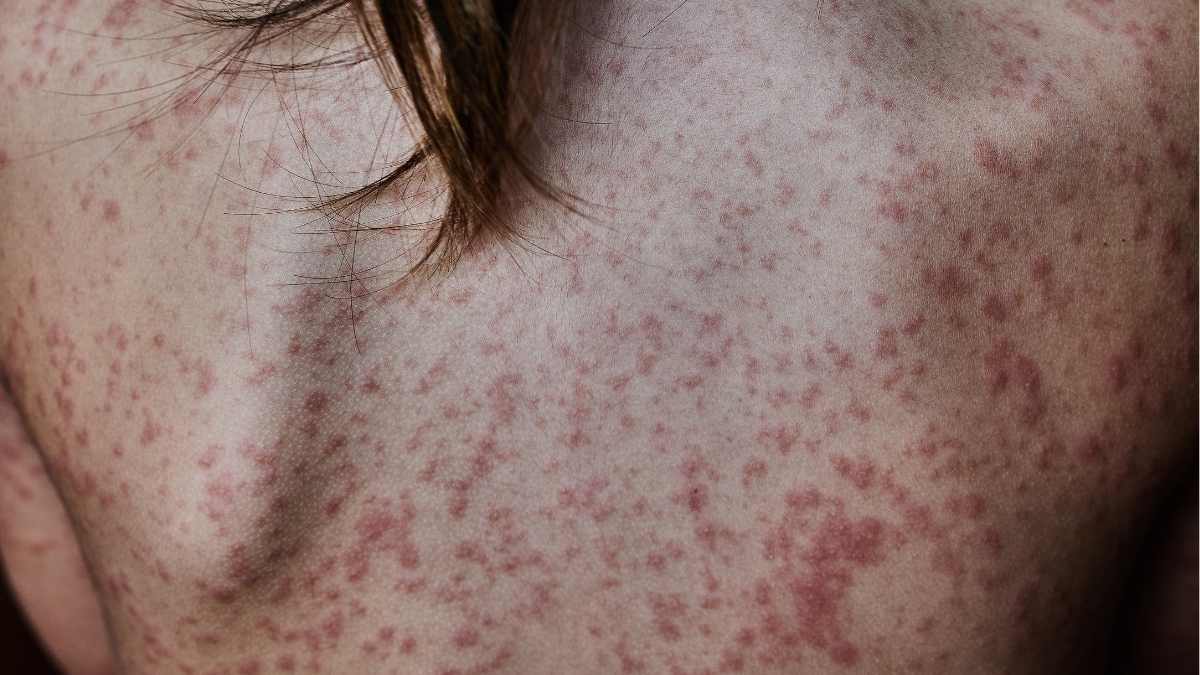
Shingles typically manifests as a painful rash that appears on one side of the body, often in a band-like pattern. The rash usually begins as red patches that develop into fluid-filled blisters. These blisters can break open, crust over, and eventually heal over a period of two to four weeks. Pain, itching, and burning sensations often accompany the rash, which can be quite severe. The initial symptoms may also include fever, headache, and fatigue, which can further complicate the clinical picture.
The visual characteristics of shingles are distinct, yet they can sometimes mimic other skin conditions. The rash usually follows the path of a nerve, appearing in a localized area rather than spreading across the body. This dermatomal distribution is a hallmark of shingles, differentiating it from other rashes that may be more generalized. The presence of blisters that evolve into crusts is a key indicator, as insect bites typically do not exhibit such a progression.
In some cases, shingles may present with atypical symptoms, especially in individuals with weakened immune systems. This can lead to a more generalized rash that may not follow the typical dermatomal pattern, making it even more challenging to distinguish from insect bites or other dermatological conditions. Recognizing these variations is crucial for healthcare providers to ensure proper diagnosis and treatment.
Additionally, the timing of the rash’s appearance in relation to other symptoms can provide clues. Shingles often follows a prodromal phase characterized by localized pain or tingling in the affected area, which can precede the rash by several days. This phase is not commonly associated with insect bites, which typically appear without prior warning.
Distinguishing Shingles from Insect Bites: A Clinical Perspective
From a clinical standpoint, distinguishing shingles from insect bites requires careful examination of the rash and consideration of accompanying symptoms. Insect bites usually present as small, raised welts that may be itchy and red, often clustered in groups. They do not typically follow a dermatomal pattern and are usually not associated with significant pain or systemic symptoms like fever.
One of the primary differentiators is the pain intensity associated with shingles. Patients often report a burning or sharp pain that can be debilitating, whereas insect bites are generally less painful and more itchy. This pain can persist even after the rash has healed, a condition known as postherpetic neuralgia, which is not a feature of insect bites.
Furthermore, the evolution of the rash is another critical factor. Shingles blisters progress through distinct stages, starting from red patches to fluid-filled vesicles, and finally to crusts. In contrast, insect bites may develop into pustules or may simply remain as red, swollen areas without the blistering stage. A thorough patient history regarding prior chickenpox infection can also provide essential context; shingles occurs only in individuals who have had chickenpox, while insect bites can affect anyone.
Healthcare providers may also utilize diagnostic tests, such as polymerase chain reaction (PCR) testing or direct fluorescent antibody tests, to confirm the presence of the varicella-zoster virus. These tests can help clarify the diagnosis when the clinical presentation is ambiguous, ensuring that patients receive appropriate care.
Common Misconceptions: Shingles vs. Bug Bites Explained
There are several misconceptions surrounding the appearance and nature of shingles that can lead to confusion. One common belief is that shingles can only occur in older adults; however, it can affect individuals of any age who have had chickenpox. This misconception can result in younger patients being misdiagnosed when they present with shingles-like symptoms.
Another misconception is that shingles is contagious in the same way as chickenpox. While the virus can be transmitted to someone who has never had chickenpox, it does not spread through casual contact. Instead, it can only be contracted through direct contact with the fluid from shingles blisters. This misunderstanding can lead to unnecessary anxiety and stigmatization of individuals with shingles.
Additionally, many people believe that all rashes that itch or are red are insect bites. This oversimplification can result in overlooking more serious conditions, including shingles, which may require medical intervention. Educating patients on the specific characteristics of shingles versus insect bites can help reduce misdiagnosis and promote timely treatment.
Lastly, there is a tendency to underestimate the importance of early intervention for shingles. Some individuals may dismiss their symptoms as minor skin irritations, delaying necessary medical care. Recognizing the urgency of shingles treatment is crucial in preventing complications such as postherpetic neuralgia.
Diagnostic Criteria for Identifying Shingles Rash Accurately
Accurate diagnosis of shingles involves a combination of clinical evaluation and patient history. Healthcare providers typically start with a physical examination of the rash, looking for the characteristic features of shingles, such as the dermatomal distribution and the progression from red patches to blisters. A detailed patient history is also vital, particularly regarding previous chickenpox infections.
In cases where the clinical presentation is unclear, laboratory tests can aid in diagnosis. PCR testing is the gold standard for identifying the varicella-zoster virus and can provide definitive results. Direct fluorescent antibody tests can also be utilized to confirm the presence of the virus in skin lesions.
Healthcare providers may also consider the patient’s overall health and immunization history. Individuals with weakened immune systems or those who have not received the shingles vaccine may be at higher risk for developing shingles and experiencing more severe symptoms. Understanding these risk factors can guide healthcare providers in their diagnostic approach.
It is also important to differentiate shingles from other conditions that can present similarly, such as herpes simplex virus infections, contact dermatitis, or even certain bacterial infections. A comprehensive differential diagnosis is essential to ensure that patients receive the correct treatment and avoid complications associated with misdiagnosis.
Treatment Options for Shingles: Addressing Misdiagnosis Risks
Treatment for shingles primarily focuses on alleviating symptoms and reducing the duration of the outbreak. Antiviral medications, such as acyclovir, valacyclovir, or famciclovir, are most effective when initiated within 72 hours of rash onset. These medications can help shorten the duration of the rash and reduce the risk of complications. Pain management is also a critical component of treatment, often involving the use of analgesics or corticosteroids.
Misdiagnosis can lead to inappropriate treatments, such as antihistamines for presumed insect bites, which may not address the underlying viral infection. This highlights the importance of accurate diagnosis to ensure that patients receive the most effective care. In some cases, patients may require additional interventions, such as topical treatments for pain relief or even nerve blocks for severe pain.
Education plays a vital role in the management of shingles. Patients should be informed about the nature of the condition, potential complications, and the importance of early treatment. Providing resources and support can empower patients to seek timely medical attention and adhere to treatment protocols.
In addition to antiviral medications, the shingles vaccine is an important preventive measure. Vaccination can significantly reduce the risk of developing shingles and its associated complications. Encouraging vaccination among eligible populations is a key public health strategy to mitigate the impact of shingles.
When to Seek Medical Advice: Shingles and Bug Bite Concerns
Determining when to seek medical advice can be challenging for individuals experiencing a rash that may resemble shingles or insect bites. If a rash is accompanied by severe pain, especially if it follows a dermatomal pattern, it is crucial to seek medical attention promptly. Early intervention can lead to better outcomes and reduce the risk of complications.
Individuals should also be vigilant for other concerning symptoms, such as fever, chills, or a general feeling of unwellness, which may indicate a more serious condition. If the rash worsens or does not respond to over-the-counter treatments, it is advisable to consult a healthcare provider. Persistent symptoms warrant further evaluation to rule out shingles or other underlying conditions.
In cases where there is uncertainty about the nature of the rash, it is always better to err on the side of caution. Healthcare providers can offer a thorough assessment and appropriate diagnostic tests to clarify the situation. Patients should feel empowered to seek medical advice when they are unsure about their symptoms.
Additionally, individuals with a history of chickenpox or weakened immune systems should be particularly proactive in seeking medical care if they develop any unusual rashes. Awareness of personal risk factors can guide individuals in making informed decisions about their health.
Conclusions:
Understanding the differences between shingles and insect bites is crucial for accurate diagnosis and effective treatment. By recognizing the distinct symptoms and visual characteristics of shingles, individuals can avoid misdiagnosis and the associated risks. Early intervention and appropriate management are essential in mitigating the impact of shingles and preventing complications. Education and awareness are key components in empowering patients to seek timely medical care when faced with uncertain skin conditions.
Read more:
-
Centers for Disease Control and Prevention (CDC) – Shingles (Herpes Zoster) – A comprehensive resource on shingles, including symptoms, treatment, and prevention strategies.
-
Mayo Clinic – Shingles – Detailed information on the symptoms, causes, and treatment options for shingles.
-
American Academy of Dermatology – Shingles – An overview of shingles, its symptoms, and how it differs from other skin conditions.
-
National Institute of Neurological Disorders and Stroke – Postherpetic Neuralgia – Information on complications associated with shingles, including postherpetic neuralgia.
-
WebMD – Shingles Overview – A patient-friendly guide to understanding shingles, its symptoms, and treatment options.