Introduction:
Identifying a rash can be a perplexing task, given the myriad of skin conditions that can present themselves. Rashes can vary significantly in appearance, location, and underlying causes. Understanding the basics of skin rashes, their characteristics, and potential triggers is crucial for effective identification and management. This article will delve into the various aspects of rashes, providing a comprehensive guide to help individuals recognize and respond to skin irritations appropriately.
Understanding the Basics of Skin Rashes and Their Types
Skin rashes are defined as changes in the skin’s appearance, texture, or color, often resulting from inflammation. They can manifest in various forms, including redness, swelling, and itching. Rashes can be classified into several categories, such as dermatitis, infections, urticaria, and psoriasis. Each category encompasses a range of conditions that may require different approaches for identification and treatment.
Dermatitis, for example, is an inflammatory condition that can be triggered by allergens or irritants. It often presents as red, itchy patches and can be further divided into contact dermatitis, atopic dermatitis, and seborrheic dermatitis. Infections, on the other hand, can be caused by bacteria, viruses, or fungi, leading to rashes that may be accompanied by other symptoms like fever or discharge. Understanding these classifications helps in narrowing down the potential causes of a rash.
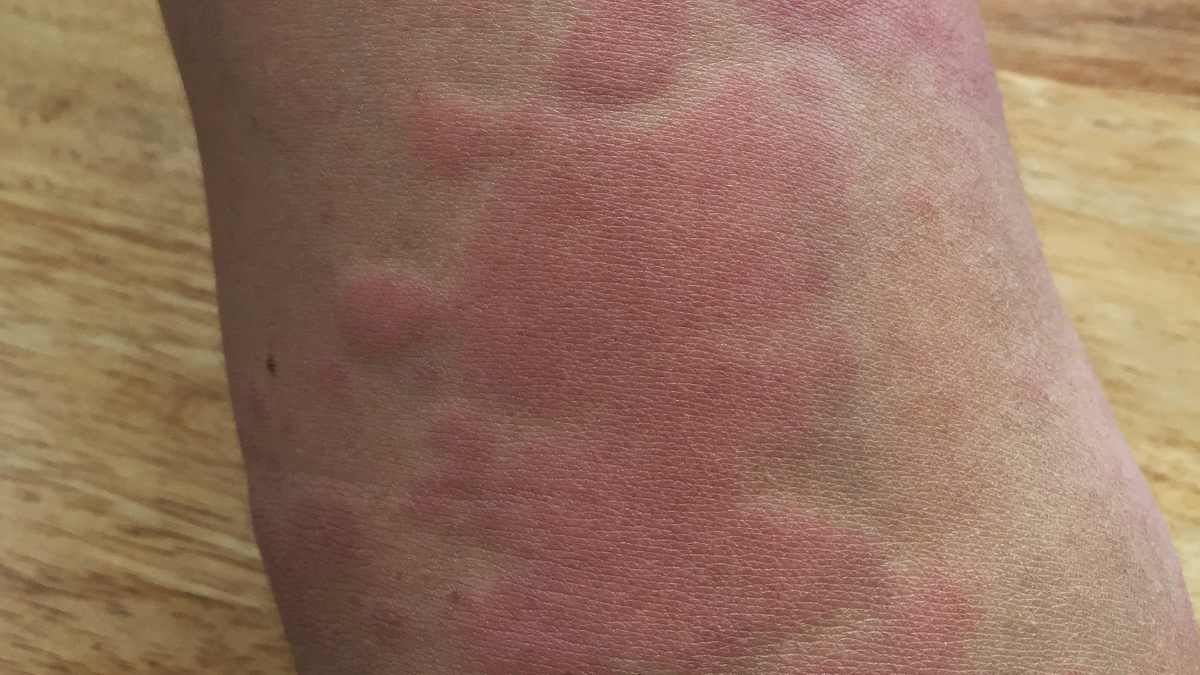
Urticaria, commonly known as hives, is characterized by raised, itchy welts that can appear suddenly and may vary in size. Psoriasis, a chronic autoimmune condition, leads to thick, red patches covered with silvery scales. Recognizing these distinct types is essential for effective management and treatment.
Lastly, rashes can also be categorized based on their duration, with acute rashes appearing suddenly and lasting for a short period, while chronic rashes persist for longer durations, often requiring ongoing medical attention.
Key Factors to Consider When Identifying a Rash
When attempting to identify a rash, several key factors must be taken into account. First and foremost is the patient’s medical history. Previous skin conditions, allergies, and family history of skin diseases can provide valuable insights into the nature of the rash. Understanding any recent changes in medication, skin care products, or environmental exposures can also aid in pinpointing the cause.
Another crucial factor is the timing and duration of the rash. Acute rashes that develop suddenly may suggest an allergic reaction or infection, while those that have persisted for weeks or months could indicate a chronic condition. Observing any patterns, such as the rash’s appearance after exposure to specific substances or environments, can further assist in identification.
The patient’s age and overall health status are also important considerations. Certain rashes are more prevalent in specific age groups, such as diaper rash in infants or shingles in older adults. Additionally, individuals with compromised immune systems may be more susceptible to certain infections that cause rashes.
Finally, the location of the rash on the body can provide clues about its cause. For instance, rashes that occur in skin folds may suggest a fungal infection, while those on exposed areas may be related to sun exposure or contact with irritants.
Visual Characteristics: Color, Texture, and Distribution
The visual characteristics of a rash are critical for identification. Color can vary widely, ranging from red and pink to brown or even purple. For instance, a bright red rash might indicate an acute inflammatory process, while a brownish hue could suggest chronic changes or post-inflammatory hyperpigmentation.
Texture is another important aspect to consider. Rashes may be smooth, scaly, raised, or blistered. For example, a scaly texture might indicate psoriasis or eczema, while a blistered rash could suggest a viral infection like chickenpox or herpes simplex. Observing these textures can help differentiate between various skin conditions.
The distribution of the rash is equally significant. Rashes can be localized to a specific area or generalized across the body. A localized rash might suggest contact dermatitis, while a widespread rash could indicate a systemic issue, such as a viral infection or an autoimmune disorder.
Additionally, the pattern of the rash can provide further diagnostic clues. For example, a ring-like pattern may suggest ringworm, while a linear pattern could indicate a reaction to a plant, such as poison ivy. Documenting these visual characteristics is essential for accurate diagnosis and treatment.
Common Causes of Rashes: Allergies, Infections, and More
Rashes can arise from a multitude of causes, with allergies being one of the most common triggers. Allergic reactions can occur due to food, medications, or environmental factors, leading to conditions like urticaria or contact dermatitis. Identifying the allergen is crucial for preventing future outbreaks and managing symptoms effectively.
Infections are another prevalent cause of rashes. Bacterial infections, such as impetigo, can lead to crusty, weeping lesions, while viral infections like measles or chickenpox result in distinctive rashes. Fungal infections, such as tinea (ringworm), can also cause rashes that are often itchy and scaly. Understanding the infectious nature of a rash is vital for determining appropriate treatment and preventing transmission.
Irritants from soaps, detergents, or environmental factors can also lead to rashes. Contact dermatitis, for example, occurs when the skin reacts to direct contact with an irritant or allergen. Identifying the source of irritation is essential for effective management and prevention of recurrence.
Lastly, autoimmune conditions such as lupus or psoriasis can manifest as rashes. These conditions often require a comprehensive approach to treatment, including medication and lifestyle modifications, to manage symptoms and prevent flare-ups. Recognizing the underlying cause of a rash is essential for effective treatment and management.
Diagnostic Approaches: When to Seek Medical Evaluation
While many rashes can be managed at home, certain situations warrant a medical evaluation. If a rash is accompanied by systemic symptoms such as fever, difficulty breathing, or swelling of the face or throat, immediate medical attention is necessary. These symptoms could indicate a severe allergic reaction or infection that requires urgent intervention.
Persistent rashes that do not respond to over-the-counter treatments or worsen over time should also be evaluated by a healthcare professional. Chronic rashes may require a more in-depth investigation, including allergy testing or skin biopsies, to determine the underlying cause and appropriate treatment.
Additionally, rashes that are painful, blistering, or associated with significant discomfort should be assessed by a medical professional. These characteristics may indicate a more serious condition that requires specialized treatment.
Finally, individuals with underlying health conditions or compromised immune systems should seek medical advice for any new or unusual rashes. Early intervention can help prevent complications and ensure appropriate management of the condition.
Treatment Options: Managing Symptoms and Underlying Causes
The treatment of rashes varies significantly depending on the underlying cause. For allergic reactions, antihistamines and topical corticosteroids are commonly used to alleviate symptoms such as itching and inflammation. Identifying and avoiding the allergen is crucial for long-term management.
In cases of infections, the treatment approach will depend on the causative agent. Bacterial infections may require antibiotics, while viral infections typically resolve on their own, with supportive care to manage symptoms. Fungal infections often necessitate antifungal medications, either topical or systemic, depending on the severity.
For chronic conditions like psoriasis or eczema, a combination of lifestyle modifications, topical treatments, and systemic therapies may be required. Moisturizers, corticosteroids, and immunosuppressive agents are commonly used to manage flare-ups and maintain skin health.
In addition to pharmacological treatments, lifestyle changes such as stress management, dietary adjustments, and proper skin care can play a significant role in preventing rashes and managing symptoms. Regular follow-ups with a healthcare provider can help monitor the condition and adjust treatment plans as necessary.
Conclusions:
Identifying a rash requires careful consideration of various factors, including medical history, visual characteristics, and potential causes. Understanding the nuances of different types of rashes, along with their triggers and treatments, can empower individuals to seek appropriate care when necessary. While many rashes can be managed at home, recognizing when to consult a healthcare professional is crucial for effective treatment and prevention of complications.
Read more
- American Academy of Dermatology – Skin Rashes – A comprehensive resource on various skin rashes, their causes, and treatments.
- Mayo Clinic – Skin Rash – Detailed information on skin rashes, including symptoms, causes, and when to seek medical help.
- Cleveland Clinic – Skin Rashes – An overview of skin rashes, their types, and associated conditions.
- WebMD – Skin Rash Symptoms and Causes – A user-friendly guide to understanding skin rashes and their management.
- National Eczema Association – Eczema and Rashes – A resource focused on eczema, its triggers, and effective management strategies.