Se hai un abbonamento attivo ACCEDI QUI
Introduction:
Internal shingles, or herpes zoster, is a viral infection that can lead to a variety of symptoms, primarily affecting the skin and nerves. However, its presentation can sometimes overlap with other medical conditions, leading to diagnostic confusion. Understanding the clinical presentation of internal shingles and recognizing conditions that may mimic its symptoms is crucial for accurate diagnosis and effective treatment. This article will explore the clinical features of internal shingles, common conditions that may be mistaken for it, distinguishing characteristics, diagnostic challenges, the importance of differential diagnosis, and the treatment implications of misdiagnosing this condition.
Understanding Internal Shingles: Clinical Presentation Overview
Internal shingles is caused by the reactivation of the varicella-zoster virus, which remains dormant in the nervous system after a person has had chickenpox. The clinical presentation of internal shingles typically includes localized pain, burning sensations, and a characteristic rash that usually appears on one side of the body. The pain often precedes the rash by several days, which can lead to confusion in diagnosis. Patients may also experience systemic symptoms such as fever, fatigue, and headaches.
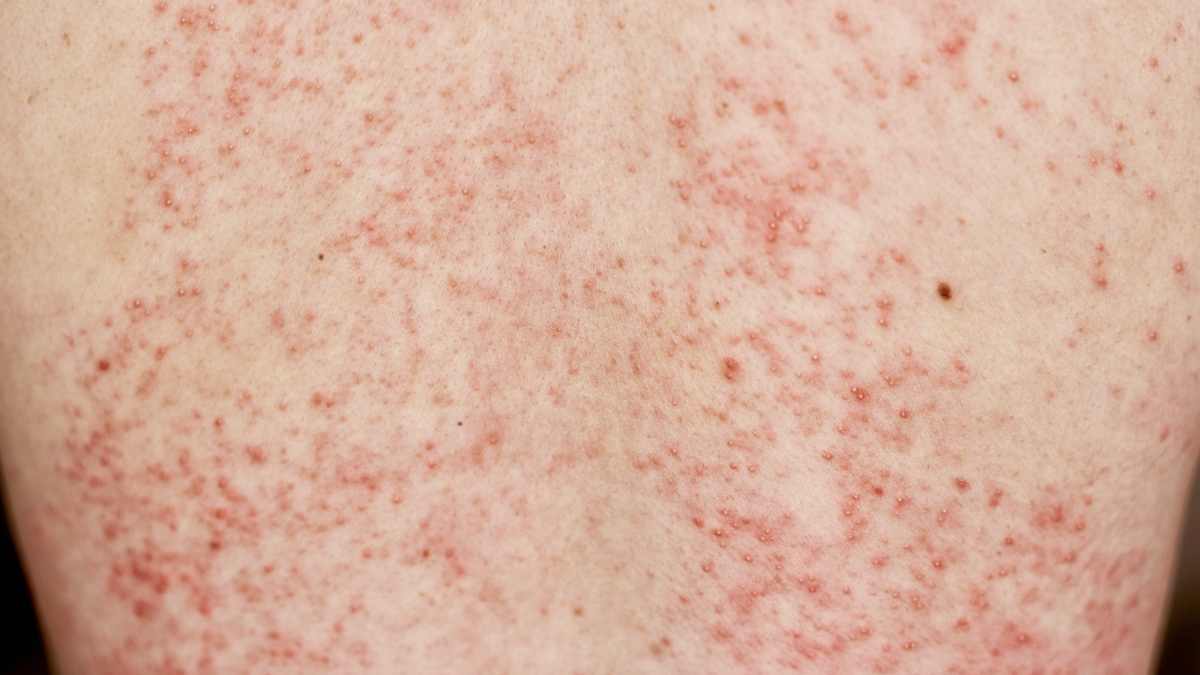
The rash associated with internal shingles generally presents as clusters of vesicles that eventually crust over. This rash is often accompanied by dermatomal distribution, meaning it follows the path of a specific nerve root. The pain associated with shingles can be severe and is often described as a sharp, stabbing sensation. This discomfort can persist even after the rash has resolved, leading to a condition known as postherpetic neuralgia.
In addition to the skin manifestations, internal shingles can affect other organ systems, particularly in immunocompromised individuals. This may lead to complications such as pneumonia, encephalitis, or even hepatitis. Understanding these potential complications is essential for healthcare providers to ensure comprehensive patient care.
Overall, the clinical presentation of internal shingles is multifaceted, making it imperative for clinicians to be aware of its symptoms and potential complications to facilitate timely and appropriate management.
Common Conditions Mimicking Internal Shingles Symptoms
Several medical conditions can mimic the symptoms of internal shingles, leading to misdiagnosis and inappropriate treatment. One common condition is herpes simplex virus (HSV) infection, which can present with similar vesicular lesions and localized pain. However, HSV typically affects the oral or genital regions, and the distribution pattern differs from that of shingles.
Another condition that may be mistaken for internal shingles is contact dermatitis, which can cause localized skin irritation and pain. This condition is often due to an allergic reaction or irritant exposure, and while it may present with vesicular lesions, the absence of dermatomal distribution can help differentiate it from shingles.
Fibromyalgia is another condition that can mimic the pain associated with internal shingles. Patients with fibromyalgia often experience widespread pain, fatigue, and sleep disturbances, which can be mistaken for the systemic symptoms of shingles. However, the absence of a rash and the presence of tender points in fibromyalgia can help distinguish the two conditions.
Lastly, gastrointestinal disorders, such as pancreatitis or peptic ulcers, can present with abdominal pain that may be confused with the visceral pain associated with internal shingles. A thorough clinical evaluation and appropriate imaging studies can aid in differentiating these conditions.
Distinguishing Features of Internal Shingles vs. Other Disorders
To accurately diagnose internal shingles, it is essential to recognize its distinguishing features compared to other disorders. One of the most significant characteristics is the dermatomal distribution of the rash and pain. Unlike other conditions that may present with pain or rashes, shingles typically follows the path of a single nerve root, making it unique in its presentation.
The prodromal phase of internal shingles, characterized by localized pain and discomfort before the appearance of the rash, is another distinguishing feature. This phase can last from a few days to a week and is not commonly seen in other conditions. Patients may report intense itching or burning sensations in the affected area, which can serve as an early warning sign of the impending rash.
The vesicular rash that develops during the course of shingles is also a key differentiator. The vesicles are usually filled with clear fluid and can become crusted over as they heal. In contrast, other conditions such as HSV infections may present with different types of lesions, and contact dermatitis may show more diffuse erythema without vesicular formation.
Finally, the presence of postherpetic neuralgia following the resolution of the rash is a unique feature of internal shingles. This chronic pain condition can persist for months or even years, significantly impacting a patient’s quality of life. Other conditions do not typically lead to such prolonged pain following resolution.
Diagnostic Challenges: Misinterpretation of Shingles Symptoms
The diagnosis of internal shingles can be challenging due to the overlapping symptoms with other medical conditions. Clinical judgment plays a crucial role in differentiating shingles from other disorders, and misinterpretation can lead to significant delays in treatment. Healthcare providers must be vigilant in recognizing the signs and symptoms of shingles, particularly in atypical presentations.
One common diagnostic challenge is the atypical presentation of shingles in immunocompromised patients. These individuals may not exhibit the classic vesicular rash, making it difficult to identify the condition. Instead, they may present with systemic symptoms or complications, which can lead to misdiagnosis as other viral infections or even bacterial infections.
Moreover, the timing of symptom onset can complicate the diagnosis. Patients may seek medical attention for pain or discomfort before the rash appears, leading to confusion regarding the underlying cause. In such cases, a detailed patient history and physical examination are essential to guide the diagnostic process.
Finally, the availability of rapid diagnostic tests can also influence the accuracy of shingles diagnosis. While polymerase chain reaction (PCR) testing can confirm the presence of the varicella-zoster virus, not all healthcare settings have access to this technology. Therefore, relying solely on clinical presentation may lead to misdiagnosis, emphasizing the need for a comprehensive approach to patient evaluation.
Importance of Differential Diagnosis in Shingles Cases
The importance of differential diagnosis in shingles cases cannot be overstated. Accurate identification of internal shingles is crucial for initiating appropriate treatment and preventing complications. Misdiagnosis can lead to unnecessary treatments, prolonged suffering, and increased healthcare costs.
A thorough differential diagnosis allows healthcare providers to consider a wide range of conditions that may present with similar symptoms. By evaluating the patient’s history, physical examination findings, and potential risk factors, clinicians can narrow down the list of possible diagnoses. This process is particularly important in cases where patients have atypical presentations or underlying health conditions that may complicate the clinical picture.
In addition, understanding the potential complications associated with misdiagnosis is vital. For instance, untreated shingles can lead to postherpetic neuralgia, which can significantly affect a patient’s quality of life. Early recognition and treatment can mitigate these risks and improve patient outcomes.
Furthermore, a comprehensive differential diagnosis can also assist in identifying coexisting conditions. Patients with shingles may have other underlying health issues that require attention, and addressing these concurrently can lead to more effective overall management.
Treatment Implications of Misdiagnosing Internal Shingles
Misdiagnosing internal shingles can have significant treatment implications. If shingles is mistaken for another condition, the patient may receive inappropriate therapies that do not address the underlying viral infection. For example, prescribing antibiotics for a suspected bacterial infection will not alleviate the symptoms of shingles and may delay appropriate antiviral treatment.
The timely initiation of antiviral therapy is essential for managing internal shingles effectively. Antiviral medications, such as acyclovir, can reduce the severity and duration of symptoms when started early in the course of the illness. Misdiagnosis can lead to delays in treatment, increasing the risk of complications such as postherpetic neuralgia.
Moreover, the management of pain associated with shingles is another critical aspect that can be affected by misdiagnosis. If the pain is attributed to a different condition, the patient may not receive the appropriate analgesics or adjunctive therapies needed to manage their discomfort effectively. This can lead to prolonged suffering and decreased quality of life.
Lastly, understanding the potential for complications associated with shingles is vital for guiding treatment decisions. If a healthcare provider misinterprets the symptoms as benign, they may overlook the need for further evaluation and monitoring for complications. This underscores the importance of accurate diagnosis and the need for ongoing education for healthcare professionals regarding the clinical features of internal shingles.
Conclusions:
In conclusion, internal shingles presents a complex clinical picture that can be easily mistaken for other medical conditions. Recognizing the distinguishing features of internal shingles, understanding common mimicking conditions, and addressing the diagnostic challenges are essential for accurate diagnosis and effective treatment. The implications of misdiagnosis can significantly impact patient care, making differential diagnosis a critical component of managing shingles cases. By prioritizing accurate identification and timely intervention, healthcare providers can improve outcomes for patients affected by this viral infection.
Read more
-
Centers for Disease Control and Prevention (CDC) – Shingles: A comprehensive overview of shingles, its causes, symptoms, and prevention strategies.
-
Mayo Clinic – Shingles (Herpes Zoster): Detailed information on shingles, including symptoms, causes, risk factors, and treatment options.
-
National Institute of Neurological Disorders and Stroke – Postherpetic Neuralgia: An informative resource on postherpetic neuralgia, a common complication of shingles.
-
American Academy of Dermatology – Shingles: A patient-focused resource detailing the signs, symptoms, and treatment of shingles.
-
WebMD – Shingles Symptoms and Treatment: An accessible overview of shingles, including symptoms, treatment options, and prevention strategies.