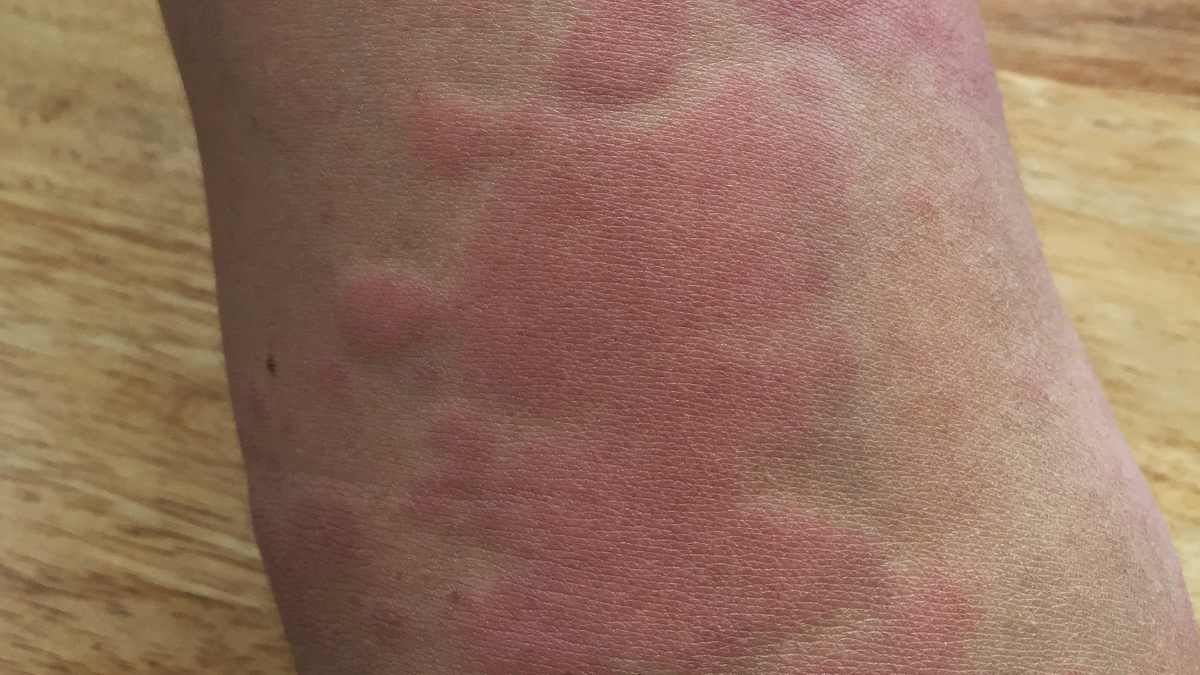
Introduction:
Lupus is a complex autoimmune disease that can affect various parts of the body, including the skin. One of the hallmark symptoms of lupus is the skin rash, which can vary significantly in appearance and severity. Understanding what a lupus skin rash looks like is crucial for early diagnosis and effective management of the condition. This article delves into the characteristics of lupus skin rashes, differentiates them from other skin conditions, and discusses diagnostic and treatment options available for those affected.
Understanding Lupus: An Overview of the Condition
Lupus, specifically systemic lupus erythematosus (SLE), is an autoimmune disorder where the immune system mistakenly attacks healthy tissues, leading to inflammation and damage. This condition can affect multiple organ systems, including the skin, joints, kidneys, and heart. The exact cause of lupus remains unclear, but it is believed to involve a combination of genetic, environmental, and hormonal factors.
Symptoms of lupus can vary widely among individuals, making it a challenging condition to diagnose. Common manifestations include fatigue, joint pain, and skin rashes. The skin involvement in lupus is particularly significant, as it can serve as an indicator of disease activity and flare-ups. Recognizing the various types of skin rashes associated with lupus is essential for patients and healthcare providers alike.
Lupus predominantly affects women, particularly those of childbearing age, although it can occur in men and children as well. The disease often presents in a relapsing-remitting pattern, with periods of exacerbation followed by remission. Understanding the systemic nature of lupus is vital for managing the disease effectively, as skin rashes may be just one aspect of a broader clinical picture.
Ultimately, lupus is a lifelong condition that requires ongoing monitoring and management. Awareness of its manifestations, particularly skin rashes, can help patients seek timely medical intervention and improve their quality of life.
Identifying Lupus Skin Rash: Key Characteristics
Lupus skin rashes can manifest in various forms, but they typically share some common characteristics. One of the most recognizable features is the butterfly rash, which appears across the cheeks and nose, resembling the shape of a butterfly. This rash is often erythematous and may be accompanied by scaling or flaking.
In addition to the butterfly rash, lupus can cause other types of skin lesions, including discoid rashes, which are circular, red, and scaly patches that can appear on the face, scalp, or other areas of the body. These lesions can be persistent and may lead to scarring if not treated appropriately.
Another key characteristic of lupus skin rashes is their tendency to worsen with sun exposure, a phenomenon known as photosensitivity. Patients may notice that their rashes become more pronounced or new rashes develop after spending time in the sun. This sensitivity to ultraviolet (UV) light is a crucial aspect of managing lupus, as it can trigger flare-ups of both skin and systemic symptoms.
It is important to note that the appearance of lupus skin rashes can vary significantly between individuals. Some may experience mild rashes that are barely noticeable, while others may have severe and extensive lesions. Understanding these characteristics is essential for patients and healthcare providers to identify and manage lupus effectively.
Common Types of Lupus Skin Rashes Explained
The butterfly rash is perhaps the most iconic representation of lupus. It typically appears as a red or purplish rash across the cheeks and bridge of the nose, often sparing the nasolabial folds. This rash can be itchy and may worsen with sun exposure. While it is not exclusive to lupus, its presence can be a strong indicator of the disease.
Discoid lupus erythematosus (DLE) is another common skin manifestation of lupus. DLE lesions are typically round, raised, and scaly, and they can occur on the face, scalp, and other sun-exposed areas. Unlike the butterfly rash, discoid lesions can lead to scarring and hair loss if they develop on the scalp.
Subacute cutaneous lupus erythematosus (SCLE) is characterized by red, scaly patches that may resemble psoriasis. These lesions often appear on sun-exposed areas and can be triggered by UV light. SCLE is notable for its potential to resolve without scarring, unlike discoid lesions.
Finally, lupus can also cause a variety of other skin changes, including vasculitis, which may present as small red or purple spots (petechiae) due to bleeding under the skin. These manifestations highlight the importance of recognizing the diverse presentations of lupus skin rashes for accurate diagnosis and management.
Distinguishing Lupus Rashes from Other Skin Conditions
Differentiating lupus skin rashes from other dermatological conditions can be challenging due to overlapping features. For instance, the butterfly rash may resemble rashes seen in conditions like rosacea or seborrheic dermatitis. Careful clinical evaluation, including patient history and symptom assessment, is essential for accurate diagnosis.
Discoid lupus lesions can be confused with psoriasis or eczema due to their scaly appearance. However, the distribution of these rashes and their response to treatment can provide valuable clues. For example, discoid lesions are more likely to be persistent and can lead to scarring, while psoriasis typically presents with well-defined plaques and may respond to topical corticosteroids.
Subacute cutaneous lupus erythematosus can mimic other conditions such as drug-induced rashes or certain types of eczema. The presence of systemic symptoms, such as joint pain or fatigue, alongside skin manifestations can help differentiate lupus from these other conditions.
In some cases, a skin biopsy may be necessary to confirm the diagnosis. Histological examination can reveal specific changes associated with lupus, such as interface dermatitis and the presence of immune complexes. Understanding these distinctions is crucial for effective management and treatment of lupus and its skin manifestations.
Diagnostic Approaches for Lupus Skin Manifestations
Diagnosing lupus skin rashes involves a comprehensive approach that includes a detailed medical history, physical examination, and laboratory tests. Physicians often begin by assessing the patient’s symptoms, including the appearance and location of rashes, as well as any associated systemic symptoms such as joint pain or fatigue.
Laboratory tests play a critical role in the diagnostic process. Common tests include antinuclear antibody (ANA) testing, which is positive in a significant number of lupus patients. Additional specific autoantibody tests, such as anti-dsDNA and anti-Smith antibodies, can further support the diagnosis.
A skin biopsy may be performed to obtain a definitive diagnosis, especially when the rash’s appearance is atypical or when distinguishing lupus from other dermatological conditions. Histopathological examination can reveal characteristic features of lupus, aiding in the diagnostic process.
Collaboration between dermatologists and rheumatologists is often beneficial in managing lupus skin manifestations. This multidisciplinary approach ensures that patients receive comprehensive care tailored to their individual needs, improving overall outcomes.
Treatment Options for Managing Lupus Skin Rashes
Managing lupus skin rashes typically involves a combination of topical and systemic treatments, depending on the severity and extent of the rashes. For mild cases, topical corticosteroids are often the first line of treatment. These medications can help reduce inflammation and alleviate symptoms such as itching and redness.
In cases where topical treatments are insufficient, systemic medications may be necessary. Antimalarial drugs, such as hydroxychloroquine, are commonly used for managing lupus skin manifestations. These medications have been shown to improve skin lesions and reduce the frequency of flare-ups.
For more severe or persistent rashes, immunosuppressive agents may be prescribed. Medications such as azathioprine or mycophenolate mofetil can help modulate the immune response and reduce skin inflammation. However, these treatments come with potential side effects and require careful monitoring.
In addition to pharmacological treatments, lifestyle modifications play a crucial role in managing lupus skin rashes. Patients are often advised to practice sun protection, such as wearing sunscreen and protective clothing, to minimize UV exposure and prevent flare-ups. Regular follow-up with healthcare providers is essential for monitoring the condition and adjusting treatment as needed.
Conclusions:
Lupus skin rashes are a significant aspect of the disease that can impact patients’ quality of life. Recognizing the various types of rashes, understanding their characteristics, and distinguishing them from other skin conditions are essential for effective management. A multidisciplinary approach involving dermatologists and rheumatologists can provide comprehensive care tailored to individual needs. With appropriate treatment and lifestyle modifications, patients can manage their skin manifestations and improve their overall well-being.
Read more
- Lupus Foundation of America – A comprehensive resource for information on lupus, including symptoms, diagnosis, and treatment options.
- American Academy of Dermatology – Provides information on skin conditions, including lupus rashes, and tips for managing skin health.
- National Institute of Arthritis and Musculoskeletal and Skin Diseases – Offers research-based information on lupus and related skin conditions.
- Mayo Clinic – Lupus – A trusted source for understanding lupus symptoms, including skin manifestations.
- Cleveland Clinic – Lupus Skin Rashes – Detailed information on various types of lupus skin rashes and their management.