Se hai un abbonamento attivo ACCEDI QUI
Introduction:
Parkinson’s disease is a progressive neurodegenerative disorder that primarily affects movement. While the hallmark symptoms include tremors, rigidity, and bradykinesia, there are several non-motor symptoms that can manifest as well. One such symptom is the Parkinson’s rash, which has garnered attention in both clinical and research settings. Understanding the characteristics, clinical implications, and management of this rash is crucial for healthcare providers and patients alike.
Understanding the Parkinson’s Rash: An Overview of Symptoms
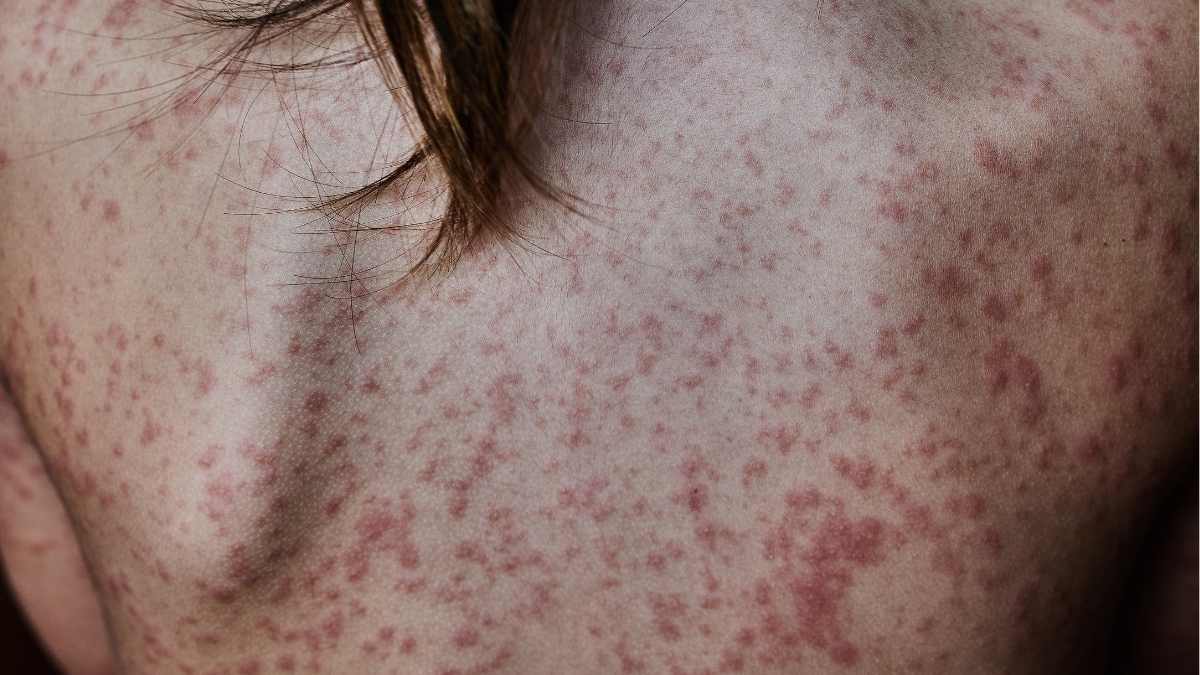
The Parkinson’s rash is often described as a distinct dermatological manifestation associated with the disease. Patients may notice changes in their skin, particularly on the face and upper body. The rash can appear as a shiny, oily, or scaly surface, often resembling seborrheic dermatitis. It may also present with redness and inflammation, contributing to discomfort for the individual. While the rash itself is not universally present in all patients with Parkinson’s, its occurrence can be indicative of the disease’s progression.
In addition to the physical appearance, the rash may also be accompanied by other symptoms, such as itching or burning sensations. These sensations can significantly affect the quality of life, leading to increased discomfort and anxiety. The rash is typically more pronounced in patients with more advanced stages of Parkinson’s disease, suggesting a correlation between disease severity and skin manifestations.
Moreover, the Parkinson’s rash can serve as a potential early warning sign for the disease. Research indicates that individuals who develop this rash may have a higher likelihood of developing Parkinson’s disease later in life. This highlights the importance of recognizing and understanding the rash as part of the broader spectrum of Parkinson’s symptoms.
Lastly, the psychological impact of the rash should not be overlooked. Patients may experience self-esteem issues due to the visible nature of the rash, leading to social withdrawal or depression. Addressing these psychological aspects is essential for comprehensive patient care.
Clinical Characteristics of the Parkinson’s Rash Presentation
Clinically, the Parkinson’s rash can be characterized by its location and morphology. It is most commonly found on the face, particularly around the eyebrows and nasolabial folds, but can also appear on the scalp and upper body. The rash may vary in color from reddish to brownish, often exhibiting a greasy or shiny appearance. This oily texture is particularly noteworthy and can help differentiate it from other skin conditions.
In terms of morphology, the rash may present as papules, plaques, or patches, and it can vary in size. The lesions can be scattered or confluent, leading to larger areas of affected skin. The presence of scales or crusting may also be observed, particularly in more severe cases. The variability in presentation can sometimes complicate the diagnosis, as it may mimic other dermatological conditions.
Additionally, the rash may not be static; it can worsen or improve over time, often influenced by factors such as stress, environmental changes, or medication adjustments. This dynamic nature can lead to fluctuations in the patient’s comfort level and may require ongoing assessment and management.
Finally, the clinical evaluation of the rash should include a thorough history and physical examination. This assessment is crucial for determining the rash’s impact on the patient’s overall health and well-being, as well as for guiding treatment options.
Distinguishing Parkinson’s Rash from Other Skin Conditions
Differentiating the Parkinson’s rash from other skin conditions is essential for accurate diagnosis and effective management. Common conditions that may resemble the Parkinson’s rash include seborrheic dermatitis, eczema, and psoriasis. Seborrheic dermatitis, in particular, shares similar characteristics, including oily patches and redness, making it a common point of confusion.
To distinguish the Parkinson’s rash, clinicians should consider the patient’s medical history and the presence of other Parkinson’s symptoms. The rash’s location, particularly its prevalence on the face and upper body, can also provide clues. Moreover, the onset and progression of the rash in conjunction with neurological symptoms can help establish a clearer diagnosis.
A skin biopsy may be warranted in ambiguous cases to rule out other dermatological conditions. Histopathological examination can reveal specific features that are characteristic of the Parkinson’s rash, aiding in the diagnostic process. Additionally, laboratory tests may be conducted to evaluate for underlying conditions that could contribute to skin changes.
Finally, patient education plays a crucial role in distinguishing the Parkinson’s rash. Patients should be informed about the characteristics of the rash and encouraged to report any changes promptly. This proactive approach can facilitate early intervention and improve patient outcomes.
Pathophysiology Behind the Development of Parkinson’s Rash
The pathophysiology of the Parkinson’s rash is not yet fully understood, but several theories have been proposed. One hypothesis suggests that the rash may be related to dysregulation of the autonomic nervous system, which is known to be affected in Parkinson’s disease. This dysregulation can lead to altered sebaceous gland activity, resulting in the oily appearance of the rash.
Another theory revolves around the role of neuroinflammation in Parkinson’s disease. Inflammation may contribute to changes in skin texture and appearance, leading to the development of the rash. The presence of inflammatory cytokines in the skin may exacerbate the condition, resulting in the characteristic symptoms observed in patients.
Additionally, the accumulation of alpha-synuclein, a protein that aggregates in the brains of Parkinson’s patients, may also play a role. Research suggests that alpha-synuclein may be involved in skin physiology, potentially leading to alterations in skin barrier function and the development of the rash.
Finally, genetic factors may also contribute to the development of the Parkinson’s rash. Certain genetic mutations associated with Parkinson’s disease may predispose individuals to skin changes, highlighting the need for further research in this area.
Diagnostic Approaches for Identifying Parkinson’s Rash
Diagnosing the Parkinson’s rash involves a comprehensive approach that includes both clinical evaluation and patient history. A detailed medical history is essential, as it can provide insights into the onset of the rash in relation to other Parkinson’s symptoms. Clinicians should inquire about the duration, progression, and associated symptoms of the rash.
A thorough physical examination is also crucial. Clinicians should assess the rash’s characteristics, including its location, color, and texture, as well as any accompanying symptoms such as itching or discomfort. This examination can help differentiate the rash from other skin conditions.
In some cases, a dermatological consultation may be beneficial, particularly if the rash is atypical or does not respond to standard treatments. Dermatologists can provide specialized expertise in diagnosing and managing skin conditions, which can aid in the overall care of the patient.
Finally, patient education is an integral part of the diagnostic process. Patients should be informed about the potential significance of the rash and encouraged to communicate any changes promptly. This collaborative approach can enhance the diagnostic process and lead to more effective management strategies.
Treatment Options and Management Strategies for Patients
Managing the Parkinson’s rash involves a multifaceted approach tailored to the individual patient’s needs. Topical treatments are often the first line of defense. Medications such as corticosteroids or antifungal creams may be prescribed to reduce inflammation and control symptoms. These treatments can help alleviate discomfort and improve the rash’s appearance.
In addition to topical therapies, moisturizers can be beneficial in managing dryness and irritation associated with the rash. Patients should be encouraged to use gentle, fragrance-free products to avoid further irritation. Regular application of moisturizers can help maintain skin integrity and reduce the severity of the rash.
Furthermore, addressing underlying factors such as stress management and lifestyle modifications can also play a significant role in managing the rash. Patients may benefit from relaxation techniques, exercise, and a balanced diet, which can contribute to overall skin health and well-being.
Finally, ongoing monitoring and follow-up are essential for patients with Parkinson’s rash. Regular assessments can help track the rash’s progression and response to treatment, allowing for timely adjustments as needed. A collaborative approach involving dermatologists, neurologists, and primary care providers can optimize patient outcomes.
Conclusions:
The Parkinson’s rash is a significant yet often overlooked symptom of Parkinson’s disease. Understanding its clinical characteristics, pathophysiology, and management strategies is crucial for healthcare providers and patients alike. By recognizing the rash as part of the broader spectrum of Parkinson’s symptoms, clinicians can provide comprehensive care that addresses both the physical and psychological aspects of the disease.
Read more:
- Parkinson’s Foundation – Skin Changes in Parkinson’s Disease – Comprehensive information on skin changes associated with Parkinson’s disease.
- National Institute of Neurological Disorders and Stroke – Parkinson’s Disease Fact Sheet – Overview of Parkinson’s disease, including symptoms and management.
- American Academy of Dermatology – Seborrheic Dermatitis – Detailed information on seborrheic dermatitis, which can resemble the Parkinson’s rash.
- Journal of the American Academy of Dermatology – Dermatological Manifestations of Parkinson’s Disease – A research article discussing various skin manifestations in Parkinson’s patients.
- PubMed – The Role of Autonomic Dysfunction in Parkinson’s Disease – A study examining the relationship between autonomic dysfunction and skin changes in Parkinson’s disease.