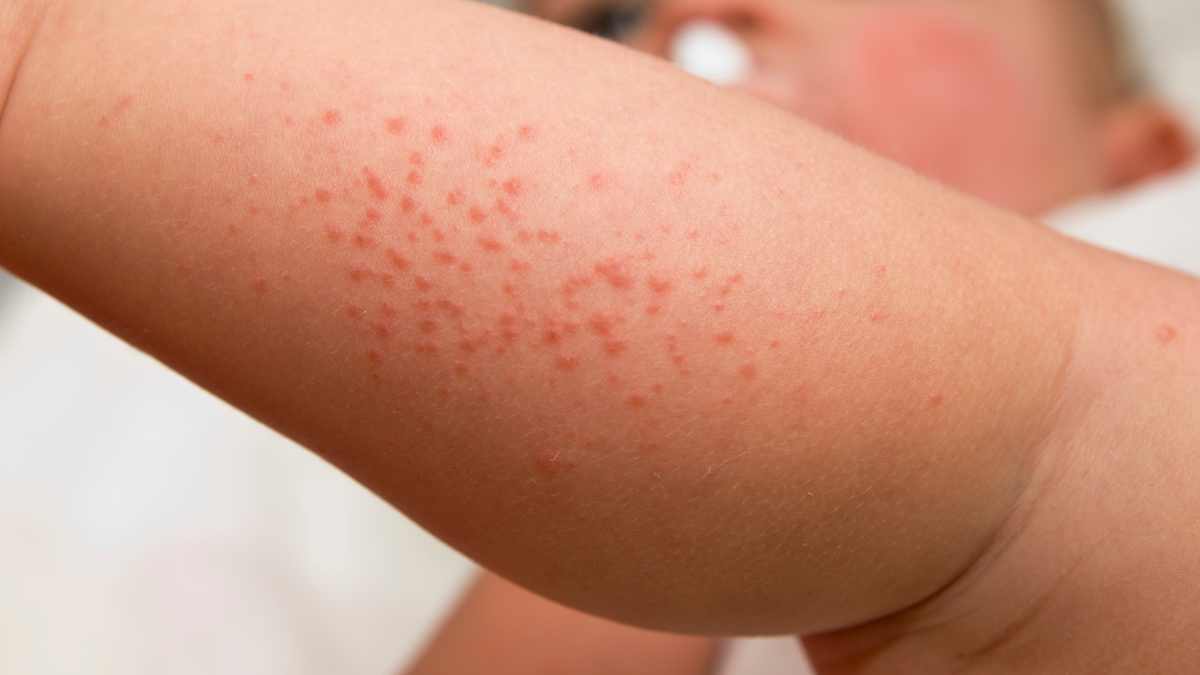
Introduction:
Vasculitis is a term that encompasses a group of disorders characterized by inflammation of the blood vessels. This inflammation can lead to a variety of symptoms, including rashes, which are often one of the most visible manifestations of the condition. Understanding what a vasculitis rash looks like is crucial for early diagnosis and treatment. This article delves into the nature of vasculitis, the types of rashes associated with it, and how these rashes can be differentiated from other skin conditions.
Understanding Vasculitis: An Overview of the Condition
Vasculitis can affect any type of blood vessel, including arteries, veins, and capillaries. The inflammation caused by vasculitis can lead to serious complications, including organ damage, as it disrupts normal blood flow. The underlying causes of vasculitis can vary widely, ranging from autoimmune diseases to infections and certain medications. In many cases, the exact cause remains unknown, leading to the classification of these conditions as idiopathic vasculitis.
The symptoms of vasculitis can vary significantly depending on the specific type and severity of the condition. While some individuals may experience systemic symptoms such as fever, fatigue, and weight loss, others may present with localized symptoms, including skin rashes. The skin manifestations of vasculitis are particularly important to recognize, as they can serve as early indicators of the disease and may prompt further investigation and treatment.
Diagnosis of vasculitis often involves a combination of clinical evaluation and laboratory tests. Medical professionals will assess the patient’s medical history, conduct physical examinations, and may order blood tests or imaging studies to confirm the diagnosis. Understanding the various types of vasculitis is essential for identifying the specific subtype affecting an individual and tailoring treatment accordingly.
Overall, early recognition and diagnosis of vasculitis are critical for preventing complications. As such, healthcare providers and patients alike must be aware of the signs and symptoms associated with this condition, particularly the rashes that can accompany it.
Common Types of Vasculitis and Their Associated Rashes
There are several types of vasculitis, each with its unique characteristics and potential skin manifestations. Granulomatosis with polyangiitis (GPA), formerly known as Wegener’s granulomatosis, is one type that can present with a rash characterized by purpura, which are small, purple spots caused by bleeding under the skin. This type of vasculitis primarily affects the respiratory tract and kidneys but can also manifest on the skin.
Microscopic polyangiitis (MPA) is another form of vasculitis that may lead to skin rashes. Patients with MPA often experience palpable purpura, which can appear as raised, reddish-purple lesions on the lower extremities. These lesions are indicative of small-vessel vasculitis and can be accompanied by systemic symptoms such as kidney dysfunction and lung involvement.
Polyarteritis nodosa (PAN) is characterized by inflammation of medium-sized arteries and can also lead to skin rashes. In PAN, patients may develop livedo reticularis, a lace-like pattern on the skin due to compromised blood flow. This condition can be serious, as it may lead to organ ischemia and other complications.
Lastly, churg-strauss syndrome, or eosinophilic granulomatosis with polyangiitis, can present with skin rashes that include papules and nodules, often accompanied by systemic symptoms such as asthma and peripheral neuropathy. Each type of vasculitis has distinct clinical features, making accurate diagnosis essential.
Key Characteristics of Vasculitis Rashes Explained
Vasculitis rashes can vary widely in appearance, but several key characteristics help differentiate them from other skin conditions. One of the most common features is purpura, which appears as small, red or purple spots on the skin. Purpura results from bleeding under the skin due to inflammation of the blood vessels, and it can be a hallmark sign of vasculitis.
Another characteristic of vasculitis rashes is the presence of ulcers or necrosis. In more severe cases, the inflammation can lead to tissue death, resulting in painful ulcers that may take time to heal. These ulcers typically occur in areas with poor blood flow, such as the legs and feet, and can significantly impact a patient’s quality of life.
Livedo reticularis is another notable feature associated with vasculitis. This condition presents as a mottled, lace-like pattern on the skin and is often seen in conditions that affect blood flow. It is crucial to recognize this pattern, as it can indicate underlying vascular compromise and the potential for more severe complications.
Finally, the distribution and symmetry of the rash can provide clues to the underlying cause. Vasculitis rashes often appear symmetrically on the body, particularly on the lower extremities. This pattern can help differentiate them from other dermatological conditions, which may present asymmetrically or in isolated patches.
Visual Differences: Vasculitis Rash vs. Other Skin Conditions
Distinguishing vasculitis rashes from other skin conditions is essential for accurate diagnosis and treatment. For instance, urticaria, or hives, is characterized by raised, itchy welts on the skin and is often associated with allergic reactions. Unlike vasculitis rashes, urticaria does not typically present with purpura or necrosis and resolves quickly with antihistamines.
Psoriasis is another skin condition that can be confused with vasculitis. Psoriasis presents as red, scaly patches that can appear anywhere on the body. However, psoriasis is primarily a chronic inflammatory skin disorder with a distinct pathophysiology, and it does not usually cause purpura or systemic symptoms associated with vasculitis.
Eczema, or atopic dermatitis, can also mimic vasculitis rashes, particularly in its acute stages. However, eczema is characterized by dry, itchy patches and does not typically involve purpura or the severe complications associated with vasculitis. Recognizing these differences is crucial for healthcare providers when evaluating patients with skin rashes.
In addition, infectious rashes, such as those caused by viral or bacterial infections, can sometimes resemble vasculitis. For example, meningococcemia can present with purpuric lesions similar to those seen in vasculitis. However, infectious rashes often have accompanying systemic symptoms like fever and malaise, which can help differentiate them from vasculitis.
Diagnostic Approaches for Identifying Vasculitis Rashes
Diagnosing vasculitis rashes involves a comprehensive approach that includes clinical evaluation, laboratory testing, and sometimes imaging studies. The first step typically involves a thorough medical history and physical examination. Healthcare providers will look for characteristic signs of vasculitis, such as purpura, ulcers, and livedo reticularis, and assess for systemic symptoms that may indicate organ involvement.
Laboratory tests play a crucial role in the diagnostic process. Blood tests can help identify markers of inflammation, such as elevated erythrocyte sedimentation rate (ESR) and C-reactive protein (CRP). Additionally, specific autoantibodies, such as anti-neutrophil cytoplasmic antibodies (ANCA), may be tested to confirm certain types of vasculitis, such as GPA and MPA.
In some cases, a skin biopsy may be necessary to confirm the diagnosis. A biopsy can reveal the presence of inflammation in the blood vessels and help differentiate vasculitis from other skin conditions. The histological examination of the biopsy sample can provide valuable information about the specific type of vasculitis affecting the patient.
Imaging studies, such as ultrasound or magnetic resonance imaging (MRI), may also be utilized to assess for vascular involvement and complications. These diagnostic approaches work together to provide a comprehensive understanding of the patient’s condition and guide appropriate treatment.
Treatment Options for Managing Vasculitis and Its Symptoms
The treatment of vasculitis is highly individualized and depends on the specific type of vasculitis, its severity, and the organs involved. The primary goal of treatment is to reduce inflammation and prevent damage to affected organs. Corticosteroids are often the first line of treatment, as they can quickly reduce inflammation and alleviate symptoms.
In cases of severe vasculitis or when corticosteroids alone are insufficient, immunosuppressive agents may be introduced. Medications such as cyclophosphamide, azathioprine, or methotrexate can help suppress the immune response and reduce inflammation. The choice of immunosuppressive therapy depends on the specific type of vasculitis and the patient’s overall health.
In addition to pharmacological treatments, supportive care is essential for managing symptoms and improving the patient’s quality of life. This may include pain management, wound care for ulcers, and physical therapy to maintain mobility. Patients may also benefit from counseling and support groups to address the emotional impact of living with a chronic condition.
Regular follow-up appointments are crucial for monitoring disease progression and treatment response. Adjustments to the treatment plan may be necessary based on the patient’s symptoms and laboratory findings. Collaborative care involving rheumatologists, dermatologists, and primary care providers is often beneficial in managing the complexities of vasculitis.
Conclusions:
Recognizing the appearance of vasculitis rashes is essential for early diagnosis and effective treatment. Understanding the various types of vasculitis, their associated skin manifestations, and the diagnostic approaches available can empower both patients and healthcare providers. Timely intervention can significantly improve outcomes and quality of life for individuals affected by this complex condition.
Read more
- Vasculitis Foundation – A comprehensive resource for information on vasculitis, including types, symptoms, and treatment options.
- National Institute of Arthritis and Musculoskeletal and Skin Diseases (NIAMS) – Offers detailed information on vasculitis and related conditions, including research updates and patient resources.
- American College of Rheumatology – Provides guidelines and educational materials on the diagnosis and management of vasculitis.
- Mayo Clinic – A trusted source for patient care and information on various health conditions, including vasculitis.
- Cleveland Clinic – Features expert articles and resources on vasculitis, its symptoms, and treatment strategies.