Introduction:
Methicillin-resistant Staphylococcus aureus (MRSA) is a type of bacteria that has become a significant public health concern due to its resistance to commonly used antibiotics. Understanding what MRSA looks like, particularly in terms of skin infections, is crucial for early identification and treatment. This article will delve into the characteristics of MRSA, its symptoms, visual signs of infection, diagnostic methods, treatment options, and preventative measures to mitigate its spread.
Understanding MRSA: An Overview of the Bacteria
MRSA is a strain of Staphylococcus aureus that has developed resistance to methicillin and other beta-lactam antibiotics. This resistance makes infections caused by MRSA more challenging to treat compared to non-resistant strains. MRSA can be found in various environments, including hospitals, schools, and gyms, and it can be transmitted through direct contact with infected individuals or contaminated surfaces.
The bacteria are classified into two main categories: healthcare-associated MRSA (HA-MRSA) and community-associated MRSA (CA-MRSA). HA-MRSA typically occurs in individuals with weakened immune systems or those undergoing invasive procedures, while CA-MRSA is more common among healthy individuals and can spread rapidly in close-contact settings. Understanding these distinctions is essential for effective prevention and control strategies.
MRSA infections can manifest in various forms, ranging from mild skin infections to severe, life-threatening conditions. The bacteria can enter the body through cuts, abrasions, or other breaks in the skin, leading to localized infections or systemic complications. The ability of MRSA to survive in harsh environments and its resistance to multiple antibiotics contribute to its persistence as a public health challenge.
As awareness of MRSA has increased, so has the need for effective education on its prevention and treatment. Health professionals and the general public must be informed about the risks associated with MRSA and the importance of hygiene practices to reduce transmission rates.
Common Symptoms Associated with MRSA Infections
The symptoms of MRSA infections can vary depending on the type and severity of the infection. In many cases, MRSA presents as a skin infection, characterized by redness, swelling, and pain at the site of infection. Patients may also experience warmth in the affected area and the presence of pus or other drainage, indicating an abscess or boil.
In more severe cases, MRSA can lead to systemic infections, which may manifest as fever, chills, and malaise. These systemic symptoms indicate that the bacteria have entered the bloodstream, potentially leading to life-threatening conditions such as sepsis. Early recognition of these symptoms is essential for prompt medical intervention.
In individuals with compromised immune systems or underlying health conditions, the symptoms may be more pronounced and can progress rapidly. It is crucial for these individuals to be vigilant about any signs of infection and seek medical attention promptly.
In summary, recognizing the common symptoms associated with MRSA infections is vital for timely diagnosis and treatment. Awareness of these symptoms can lead to quicker medical responses, potentially reducing the severity of the infection and improving patient outcomes.
Visual Characteristics of MRSA Skin Infections
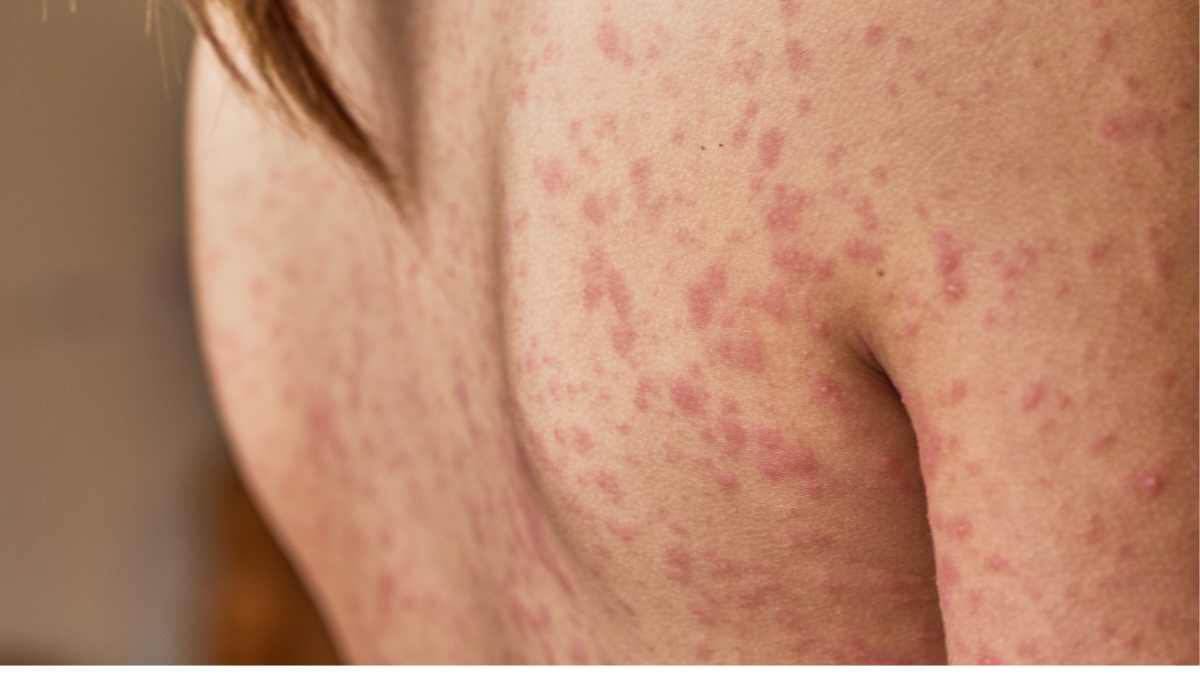
When examining MRSA skin infections, certain visual characteristics can help in identifying the presence of the bacteria. Typically, MRSA infections appear as red, swollen areas on the skin that may feel warm to the touch. As the infection progresses, these areas may develop pustules or boils, which are filled with pus and can be painful.
The skin lesions caused by MRSA can vary in size and may resemble other types of skin infections, such as cellulitis or abscesses. However, MRSA infections often have a distinctive appearance, with a well-defined border and a tendency to spread rapidly if left untreated. In some cases, the skin may also exhibit crusting or scabbing, indicating that the infection is worsening.
In addition to localized skin infections, MRSA can also cause more extensive skin conditions, such as necrotizing fasciitis, which is characterized by the rapid destruction of soft tissue. This condition requires immediate medical attention and is often accompanied by severe pain, fever, and systemic symptoms.
It is important to note that not all skin infections are caused by MRSA, and proper medical evaluation is necessary to determine the underlying cause. Visual characteristics alone cannot confirm the presence of MRSA; laboratory testing is essential for accurate diagnosis.
Diagnostic Methods for Identifying MRSA
Diagnosing MRSA infections typically involves a combination of clinical evaluation and laboratory testing. Healthcare providers begin with a thorough examination of the patient’s symptoms and medical history. If MRSA is suspected, a sample of the infected tissue or fluid may be collected for further analysis.
The most common diagnostic method for identifying MRSA is culture and sensitivity testing. In this process, the collected sample is cultured in a laboratory to determine the presence of Staphylococcus aureus and its resistance to methicillin. This testing not only confirms the diagnosis but also helps guide appropriate antibiotic therapy.
In some cases, molecular diagnostic techniques, such as polymerase chain reaction (PCR), may be employed for quicker results. PCR can detect the genetic material of MRSA in a sample, providing a rapid diagnosis that can be crucial in managing severe infections.
It is essential for healthcare providers to consider the patient’s risk factors and clinical presentation when diagnosing MRSA. Early identification is critical for effective treatment and to prevent the spread of the bacteria to others.
Treatment Options for MRSA: A Clinical Perspective
The treatment of MRSA infections depends on the severity of the infection and the patient’s overall health. For mild skin infections, drainage of abscesses may be sufficient, and antibiotics may not be necessary. However, in cases where antibiotics are required, healthcare providers typically prescribe vancomycin or daptomycin, which are effective against MRSA.
For more severe infections, particularly those that are systemic, intravenous (IV) antibiotics may be necessary. In these situations, healthcare providers may also consider using linezolid or tigecycline, which are newer antibiotics specifically designed to combat resistant strains of bacteria.
It is important to note that antibiotic resistance remains a significant concern in the treatment of MRSA. Overuse and misuse of antibiotics can lead to further resistance, making it essential for healthcare providers to follow established guidelines for antibiotic stewardship.
In addition to antibiotic treatment, supportive care may be necessary for patients with severe infections. This can include hospitalization, intravenous fluids, and monitoring for complications. A multidisciplinary approach involving infectious disease specialists may also be beneficial in managing complex cases.
Preventative Measures to Combat MRSA Spread
Preventing the spread of MRSA is crucial in both healthcare settings and the community. Hand hygiene is one of the most effective measures to reduce transmission. Regular handwashing with soap and water or the use of alcohol-based hand sanitizers can significantly decrease the risk of infection.
In healthcare settings, strict adherence to infection control protocols is essential. This includes the use of personal protective equipment (PPE), proper sterilization of medical instruments, and isolation of infected patients when necessary. Healthcare workers should also be trained to recognize and manage MRSA infections promptly.
In community settings, individuals should be educated about the importance of avoiding sharing personal items, such as towels, razors, and sports equipment, which can harbor the bacteria. Regular cleaning and disinfection of frequently touched surfaces can also help reduce the risk of transmission.
Finally, vaccination against other infections, such as influenza and pneumococcal disease, can help reduce the overall burden of illness and the likelihood of secondary infections, including MRSA. Public health campaigns aimed at raising awareness about MRSA and its prevention are essential for controlling its spread.
Conclusions:
Understanding what MRSA looks like and how it manifests in various forms is critical for effective diagnosis and treatment. By recognizing the symptoms and visual characteristics of MRSA infections, individuals and healthcare providers can respond promptly to this serious public health threat. Moreover, implementing preventative measures and adhering to treatment guidelines can significantly reduce the incidence and impact of MRSA infections.
Read more
- Centers for Disease Control and Prevention (CDC) – MRSA: Comprehensive information on MRSA, including prevention, treatment, and statistics.
- World Health Organization (WHO) – Antimicrobial Resistance: A global perspective on antimicrobial resistance, including MRSA.
- Mayo Clinic – MRSA Infections: Detailed overview of MRSA, its symptoms, causes, and treatment options.
- National Institutes of Health (NIH) – MRSA: Research findings on the seriousness of MRSA infections and their implications.
- American Academy of Dermatology – MRSA Skin Infections: Information on MRSA skin infections, including symptoms and treatment options.