Introduction:
Prozac, a widely prescribed selective serotonin reuptake inhibitor (SSRI), is primarily used to treat depression, anxiety disorders, and certain other mental health conditions. While many individuals benefit from its therapeutic effects, it is essential to be aware of potential side effects, including skin reactions. Among these, rashes can occur, prompting patients to seek clarity on their appearance and implications. This article aims to provide a comprehensive understanding of what a rash induced by Prozac may look like, its characteristics, and when to seek medical attention.
Understanding Prozac and Its Potential Side Effects
Prozac, or fluoxetine, functions by increasing serotonin levels in the brain, which can help improve mood and alleviate anxiety. As with any medication, it comes with a range of potential side effects. While many patients tolerate Prozac well, some may experience adverse reactions, including gastrointestinal disturbances, sleep changes, and skin reactions. Understanding these side effects is crucial for patients and healthcare providers alike.
Skin reactions can manifest in various forms, from mild irritations to more severe conditions. The incidence of skin rashes associated with Prozac is relatively low compared to other side effects, but they can still occur. Recognizing the signs of these reactions is vital for timely intervention and management. Patients should be informed about the possibility of skin reactions when prescribed Prozac, allowing them to monitor their health closely during treatment.
In addition to rashes, other skin-related side effects may include itching, hives, or more severe allergic reactions. Awareness of these potential issues can help patients distinguish between common side effects and more serious conditions. It is essential to maintain open communication with healthcare providers regarding any changes in skin condition while on Prozac.
Ultimately, the benefits of Prozac often outweigh the risks for many individuals. However, being informed about potential side effects, including skin reactions, is a critical aspect of patient care and safety. Patients should feel empowered to report any concerning symptoms to their healthcare provider.
Identifying Skin Reactions Associated with Prozac
Skin reactions can vary significantly in appearance and severity. Some individuals may experience mild rashes that resemble common skin irritations, while others may develop more pronounced reactions. Understanding the different types of skin reactions is essential for accurate identification and management.
Commonly reported skin reactions associated with Prozac include maculopapular rashes, urticaria (hives), and, in rare cases, more severe conditions like Stevens-Johnson syndrome. Each type of rash has distinct characteristics that can help in identifying its origin. For instance, maculopapular rashes typically present as red, raised bumps on the skin, while hives appear as welts that may itch or burn.
It is important to note that the onset of a rash may occur at any time during treatment, even after prolonged use of the medication. This unpredictability can make it challenging for patients to connect the rash with their medication. Patients should be vigilant and monitor their skin for any changes, especially after starting or adjusting their Prozac dosage.
In some cases, skin reactions may resolve on their own without discontinuing the medication. However, persistent or worsening rashes should prompt further evaluation. Understanding the nature of these skin reactions is crucial for effective management and treatment.
Characteristics of a Rash Induced by Prozac
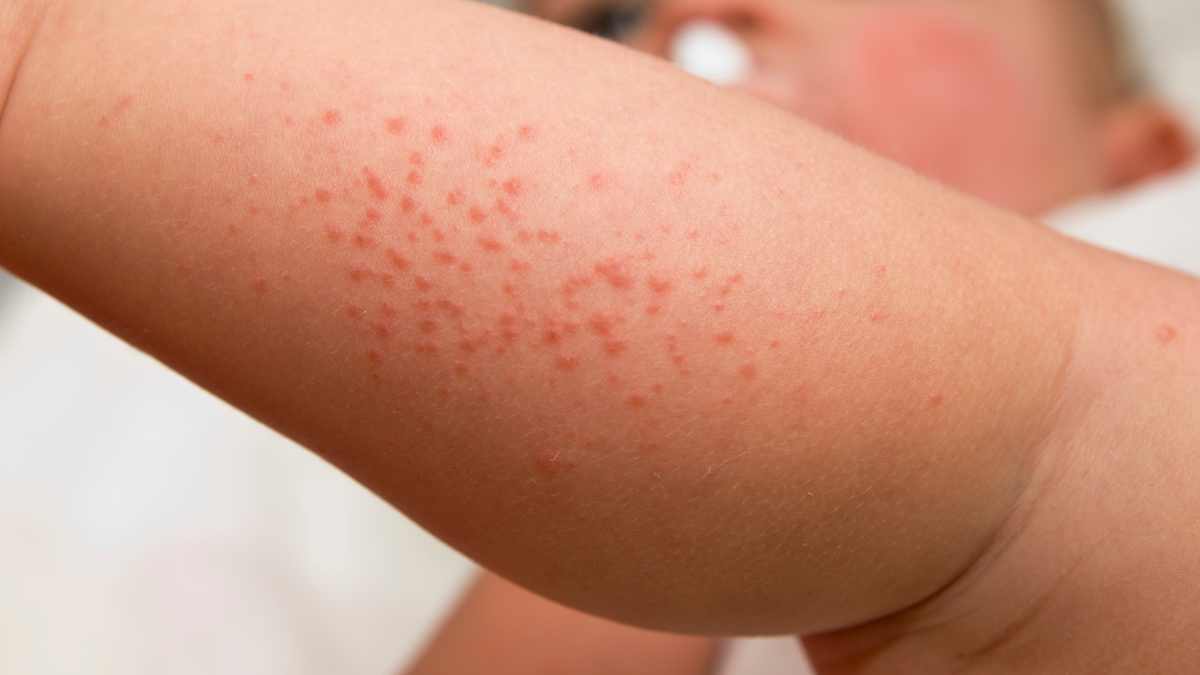
Rashes induced by Prozac can exhibit various characteristics, which may help in distinguishing them from other dermatological conditions. Typically, these rashes may present as red, raised patches or bumps on the skin. The texture can vary from smooth to rough, and they may be accompanied by itching or discomfort.
The color of the rash can range from light pink to deep red, depending on the individual’s skin tone and the severity of the reaction. In some cases, the rash may also develop blisters or pustules, indicating a more severe reaction. These characteristics can help patients and healthcare providers assess the severity of the rash and determine appropriate interventions.
Additionally, the duration of the rash can vary significantly. Some individuals may experience a transient rash that resolves within a few days, while others may have persistent symptoms requiring medical intervention. Monitoring the duration and progression of the rash is essential for effective management.
It is crucial for patients to document any accompanying symptoms, such as fever or swelling, which may indicate a more serious allergic reaction. This information can be invaluable for healthcare providers in determining the appropriate course of action.
Common Locations for Prozac-Related Skin Rashes
Prozac-related skin rashes can occur in various locations on the body, although certain areas may be more commonly affected. Typically, rashes may appear on the trunk, arms, and legs. These areas are often more exposed and prone to irritation, making them common sites for skin reactions.
In some cases, rashes may also develop on sensitive areas, such as the face or neck. These locations can be particularly concerning for patients, as facial rashes may impact self-esteem and quality of life. It is essential for patients to be aware of the potential for rashes in these visible areas and to seek prompt medical advice if they occur.
The distribution of the rash can also provide clues about its origin. For instance, a rash that is localized to a specific area may indicate contact dermatitis or an allergic reaction, while a more generalized rash may suggest a systemic response. Understanding these patterns can aid in the diagnostic process.
Ultimately, the location of the rash, combined with its characteristics, can help healthcare providers determine the best course of action for treatment. Patients should be encouraged to report any changes in skin condition, regardless of location.
Differentiating Prozac Rash from Other Skin Conditions
Differentiating a rash caused by Prozac from other skin conditions can be challenging, as many dermatological issues share similar characteristics. Common skin conditions, such as eczema, psoriasis, and contact dermatitis, may exhibit overlapping symptoms. Understanding the nuances of each condition is crucial for accurate diagnosis and treatment.
Eczema, for instance, typically presents with dry, itchy patches that may become inflamed. In contrast, a rash induced by Prozac may appear suddenly and may be accompanied by other symptoms, such as fever or malaise. Recognizing these differences can help patients and healthcare providers narrow down the potential causes of the rash.
Psoriasis, another common skin condition, is characterized by thick, scaly patches that can be itchy or painful. Unlike a Prozac rash, psoriasis is often chronic and may require long-term management. Patients should be aware of these distinctions to facilitate effective communication with their healthcare providers.
In some cases, a healthcare provider may recommend a skin biopsy or other diagnostic tests to confirm the nature of the rash. This step can be essential for ruling out other conditions and ensuring appropriate treatment. Patients should feel empowered to discuss their concerns and seek clarification on their diagnosis.
When to Seek Medical Attention for Prozac Rash
While many skin reactions may resolve without intervention, it is essential to know when to seek medical attention. Patients should be vigilant for signs of severe allergic reactions, such as difficulty breathing, swelling of the face or throat, or widespread rash. These symptoms may indicate a life-threatening condition and require immediate medical intervention.
If a rash persists for more than a few days or worsens despite home care measures, patients should consult their healthcare provider. Persistent rashes can lead to secondary infections or complications, making timely evaluation crucial. Additionally, if the rash is accompanied by systemic symptoms, such as fever or malaise, medical attention should be sought promptly.
Patients should also consider discontinuing the medication if they experience severe or intolerable skin reactions. Consulting with a healthcare provider before making any changes to medication regimens is essential. Providers can offer alternative treatment options or adjust dosages to minimize side effects.
Ultimately, open communication with healthcare providers is vital for managing any adverse reactions to Prozac. Patients should feel comfortable discussing their symptoms and concerns to ensure appropriate care.
Conclusions:
Understanding the potential skin reactions associated with Prozac is crucial for patients undergoing treatment. By recognizing the characteristics of a rash, its common locations, and how to differentiate it from other skin conditions, individuals can take proactive steps in managing their health. It is equally important to know when to seek medical attention to ensure timely intervention and prevent complications.
Read more:
- Mayo Clinic – Prozac (Fluoxetine) Overview – A comprehensive overview of Prozac, including potential side effects and patient information.
- WebMD – Prozac Side Effects – Detailed information about Prozac, including side effects and skin reactions.
- American Academy of Dermatology – Skin Rashes – An informative resource on various skin rashes and their causes.
- National Institutes of Health – Fluoxetine – A study discussing the effects and side effects of fluoxetine, including skin reactions.
- Cleveland Clinic – When to Seek Medical Attention – Guidelines on when to seek medical attention for allergic reactions, including skin rashes.