Se hai un abbonamento attivo ACCEDI QUI
Introduction:
Rheumatoid vasculitis is a serious complication of rheumatoid arthritis (RA), characterized by inflammation of the blood vessels. This condition can lead to a variety of symptoms, including skin manifestations such as rashes. Understanding the appearance and characteristics of these rashes is crucial for timely diagnosis and management. In this article, we will delve into the nature of rheumatoid vasculitis, focusing specifically on the rash associated with it, its clinical presentation, distinguishing features, diagnostic approaches, and management strategies.
Understanding Rheumatoid Vasculitis and Its Manifestations
Rheumatoid vasculitis occurs when the immune system attacks the blood vessels, leading to inflammation and damage. This condition is often associated with long-standing rheumatoid arthritis and can affect various organs, including the skin, kidneys, and nervous system. The severity of rheumatoid vasculitis can vary, with some patients experiencing mild symptoms while others may face life-threatening complications.
The skin manifestations of rheumatoid vasculitis are particularly concerning, as they can indicate systemic involvement. Patients may present with a range of dermatological symptoms, including rashes, ulcers, and necrosis. Understanding these manifestations is essential for healthcare providers to differentiate between rheumatoid vasculitis and other dermatological conditions that may present similarly.
The pathophysiology of rheumatoid vasculitis involves immune complex deposition and subsequent inflammation of the vessel walls, leading to ischemia and necrosis of the surrounding tissues. This process can result in a variety of clinical symptoms, including pain, swelling, and skin changes. Recognizing these symptoms early can significantly impact patient management and outcomes.
In summary, rheumatoid vasculitis is a serious condition that can manifest in various ways, particularly through skin rashes. Awareness of these manifestations is vital for healthcare professionals, as it aids in the early identification and treatment of this potentially debilitating complication of rheumatoid arthritis.
Clinical Presentation of Rash in Rheumatoid Vasculitis
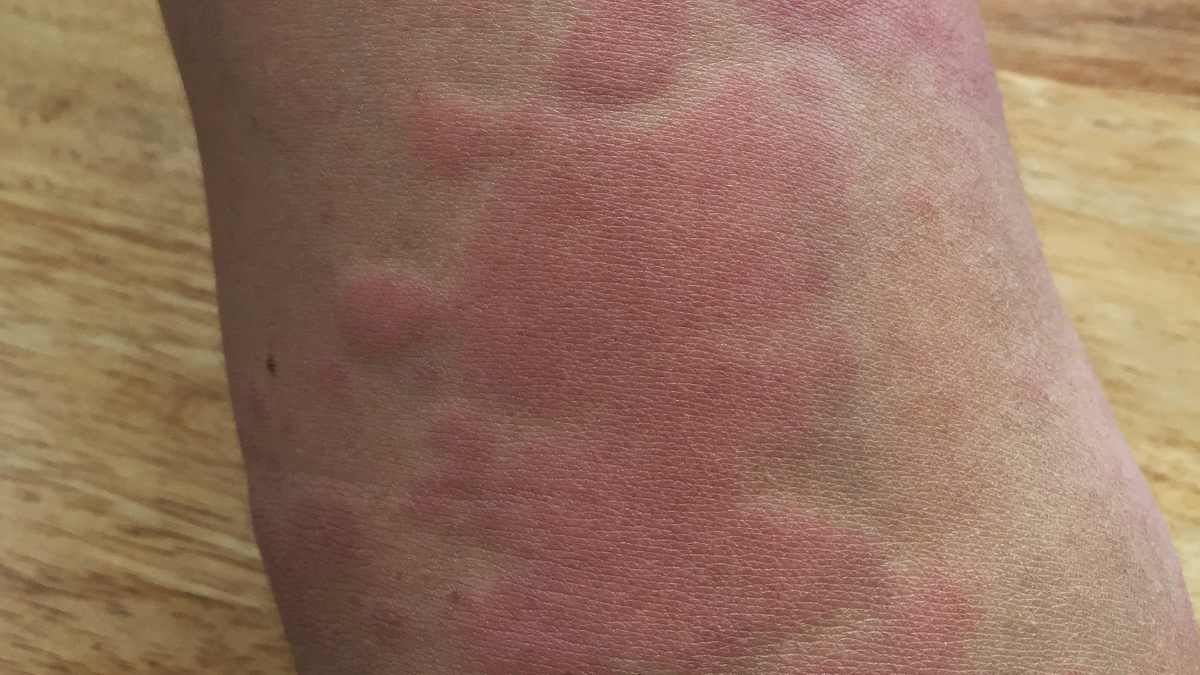
The rash associated with rheumatoid vasculitis can take several forms, often presenting as palpable purpura, which are raised, reddish-purple lesions that appear on the skin. These lesions are a result of small blood vessel inflammation and can be quite painful. They are commonly found on the lower extremities, particularly the legs and feet, but can also appear on other areas of the body.
In addition to palpable purpura, patients may experience other types of skin lesions, including ulcers and necrotic areas. These lesions can develop due to the compromised blood flow resulting from vasculitis, leading to tissue death. The presence of such lesions often indicates a more severe form of the disease and may require urgent medical attention.
Another clinical feature of the rash is its association with systemic symptoms. Patients with rheumatoid vasculitis may present with fever, malaise, and joint pain, in addition to the skin manifestations. This systemic involvement can complicate the diagnosis, as the rash may be mistaken for other conditions, such as infections or drug reactions.
In conclusion, the clinical presentation of rash in rheumatoid vasculitis is diverse, with palpable purpura being the hallmark feature. The presence of ulcers and necrotic lesions further complicates the clinical picture, often necessitating a multidisciplinary approach to management.
Common Characteristics of Rheumatoid Vasculitis Rash
Rashes associated with rheumatoid vasculitis exhibit distinct characteristics that differentiate them from other dermatological conditions. One of the most notable features is the palpable purpura, which is often described as tender, raised, and reddish-purple. These lesions typically do not blanch when pressure is applied, a key distinguishing factor.
The distribution of the rash is also significant. While purpura can appear anywhere on the body, they are most commonly found on dependent areas, such as the lower extremities. This pattern is indicative of the underlying vascular inflammation and is an important clue for clinicians in diagnosing rheumatoid vasculitis.
Another characteristic of the rash is its potential to evolve over time. Lesions may start as small spots and can coalesce into larger areas of purpura. In some cases, these lesions may progress to form ulcers or necrotic tissue, particularly in patients with severe vasculitis. The evolution of the rash can provide insight into the severity of the underlying condition.
Lastly, the presence of associated symptoms, such as joint pain and systemic signs like fever, can help clinicians assess the overall impact of the vasculitis. The combination of these characteristics is crucial for healthcare providers in forming an accurate diagnosis and developing an appropriate treatment plan.
Distinguishing Rheumatoid Vasculitis Rash from Other Rashes
Differentiating rheumatoid vasculitis rash from other skin conditions is critical for effective management. One of the primary considerations is the history of rheumatoid arthritis in the patient. A known diagnosis of RA, particularly in patients with long-standing disease, raises suspicion for vasculitis when rashes are present.
Infectious rashes, such as those caused by viral or bacterial infections, can mimic the appearance of vasculitis rash. However, infectious rashes often present with additional systemic symptoms such as fever, chills, and malaise. A thorough patient history, including recent infections or exposure, can help differentiate these conditions.
Drug reactions can also present with rashes that resemble those seen in rheumatoid vasculitis. However, drug-induced rashes typically have a more acute onset and may be associated with other symptoms such as itching or burning. A careful review of the patient’s medication history is essential in making this distinction.
Finally, other forms of vasculitis, such as cutaneous leukocytoclastic vasculitis or systemic lupus erythematosus, can present with similar rashes. Distinguishing features, such as the presence of systemic symptoms or specific laboratory findings, can aid in differentiating these conditions from rheumatoid vasculitis.
Diagnostic Approaches for Identifying Vasculitis Rash
Diagnosing a rash associated with rheumatoid vasculitis involves a comprehensive approach that includes clinical evaluation, laboratory tests, and imaging studies. A thorough history and physical examination are essential first steps. Clinicians should assess the characteristics of the rash, its distribution, and any associated symptoms.
Laboratory tests play a crucial role in confirming the diagnosis. Blood tests may reveal elevated inflammatory markers, such as C-reactive protein (CRP) and erythrocyte sedimentation rate (ESR). Additionally, specific autoantibodies, such as rheumatoid factor (RF) and anti-citrullinated protein antibodies (ACPA), can support the diagnosis of rheumatoid arthritis and its complications.
Skin biopsy is often performed to obtain a definitive diagnosis. Histopathological examination of the biopsy can reveal the characteristic findings of vasculitis, such as leukocytoclastic vasculitis or fibrinoid necrosis of the vessel walls. This information is invaluable in distinguishing rheumatoid vasculitis from other dermatological conditions.
Imaging studies, such as ultrasound or magnetic resonance imaging (MRI), may be utilized to assess the extent of vascular involvement and to evaluate for any associated complications. These diagnostic approaches collectively contribute to a comprehensive understanding of the patient’s condition and guide subsequent management.
Management Strategies for Rheumatoid Vasculitis Rash
Managing a rash associated with rheumatoid vasculitis requires a multifaceted approach, focusing on both the skin manifestations and the underlying rheumatoid arthritis. The first line of treatment often includes corticosteroids, which help reduce inflammation and alleviate symptoms. These medications can be administered topically for localized rashes or systemically for more extensive involvement.
In cases where corticosteroids alone are insufficient, immunosuppressive agents may be introduced. Medications such as methotrexate, azathioprine, or cyclophosphamide can help control the underlying autoimmune process and improve skin manifestations. The choice of immunosuppressive therapy depends on the severity of the vasculitis and the patient’s overall health status.
Additionally, supportive care measures are essential in managing the rash. This may include wound care for ulcers, pain management, and education on skin protection to prevent further injury. Regular follow-up appointments are crucial to monitor the patient’s response to treatment and adjust the management plan as necessary.
In severe cases, particularly those involving life-threatening complications, more aggressive treatments such as biologic therapies or plasmapheresis may be warranted. These advanced therapies target specific pathways in the immune response and can provide significant benefits for patients with refractory symptoms.
Conclusions:
Rheumatoid vasculitis is a complex condition that can significantly impact a patient’s quality of life. Recognizing the characteristics of the associated rash is vital for timely diagnosis and management. By understanding the clinical presentation, distinguishing features, and appropriate diagnostic and management strategies, healthcare providers can improve outcomes for patients suffering from this serious complication of rheumatoid arthritis.
Read more
- American College of Rheumatology – Offers comprehensive resources on rheumatoid arthritis and associated complications, including vasculitis.
- National Institute of Arthritis and Musculoskeletal and Skin Diseases – Provides detailed information on vasculitis and its manifestations.
- Mayo Clinic – A reliable source for patient education on rheumatoid arthritis and its complications.
- Cleveland Clinic – Features articles and resources on the management of rheumatoid arthritis and vasculitis.
- PubMed – A database of medical literature that includes research articles on rheumatoid vasculitis and its clinical features.