Se hai un abbonamento attivo ACCEDI QUI
Introduction:
Septic rash is a term that refers to a skin condition associated with systemic infection, often resulting from bacteria, viruses, or fungi. It can manifest in various ways, making it crucial for healthcare professionals and patients alike to recognize its characteristics and implications. Understanding septic rash is essential for timely diagnosis and effective treatment. This article aims to provide a comprehensive overview of septic rash, including its definition, causes, clinical presentation, differential diagnosis, diagnostic approaches, and management strategies.
Understanding Septic Rash: Definition and Overview
Septic rash is typically a sign of an underlying systemic infection, often linked to sepsis, a life-threatening condition arising from the body’s response to infection. The rash may appear as a result of the body’s inflammatory response to pathogens, leading to changes in the skin’s appearance. It is important to differentiate septic rash from other types of rashes, as it may indicate a severe medical condition requiring immediate attention.
The rash can occur in various forms, including macules, papules, vesicles, or pustules, depending on the causative agent and the individual’s immune response. In many cases, septic rash is accompanied by other systemic symptoms such as fever, chills, and malaise, which can aid in the overall assessment of the patient’s condition. Recognizing these symptoms early can significantly impact the outcome of the treatment.
Septic rash is not confined to a specific age group or demographic; it can occur in individuals of all ages, particularly those with compromised immune systems or existing health conditions. Understanding the demographics and risk factors associated with septic rash can help healthcare providers identify at-risk populations and implement preventive measures.
In summary, septic rash serves as an important clinical indicator of underlying infections. Its recognition is vital for initiating prompt treatment and preventing potential complications associated with sepsis.
Common Causes and Risk Factors of Septic Rash
Several pathogens can lead to the development of septic rash, with bacteria being the most common culprits. Staphylococcus aureus, including methicillin-resistant strains (MRSA), is frequently associated with skin infections that can progress to septic conditions. Other bacteria, such as Streptococcus pneumoniae and Escherichia coli, can also contribute to septic rash, particularly in cases of urinary tract infections or pneumonia.
Viral infections, such as those caused by the varicella-zoster virus or the herpes simplex virus, can also lead to septic rash. These viruses can trigger a systemic inflammatory response, resulting in skin manifestations that resemble a rash. Fungal infections, while less common, can also cause septic rashes, particularly in immunocompromised individuals.
Certain risk factors increase the likelihood of developing septic rash. Individuals with chronic illnesses, such as diabetes or cancer, are at a higher risk due to their weakened immune systems. Additionally, those with open wounds, invasive devices, or recent surgical procedures may be more susceptible to infections that can lead to septic rash.
Environmental factors, including poor hygiene and exposure to contaminated water or surfaces, can also contribute to the risk of septic rash. Recognizing these risk factors is essential for both prevention and early intervention in at-risk populations.
Clinical Presentation: Visual Characteristics of Septic Rash
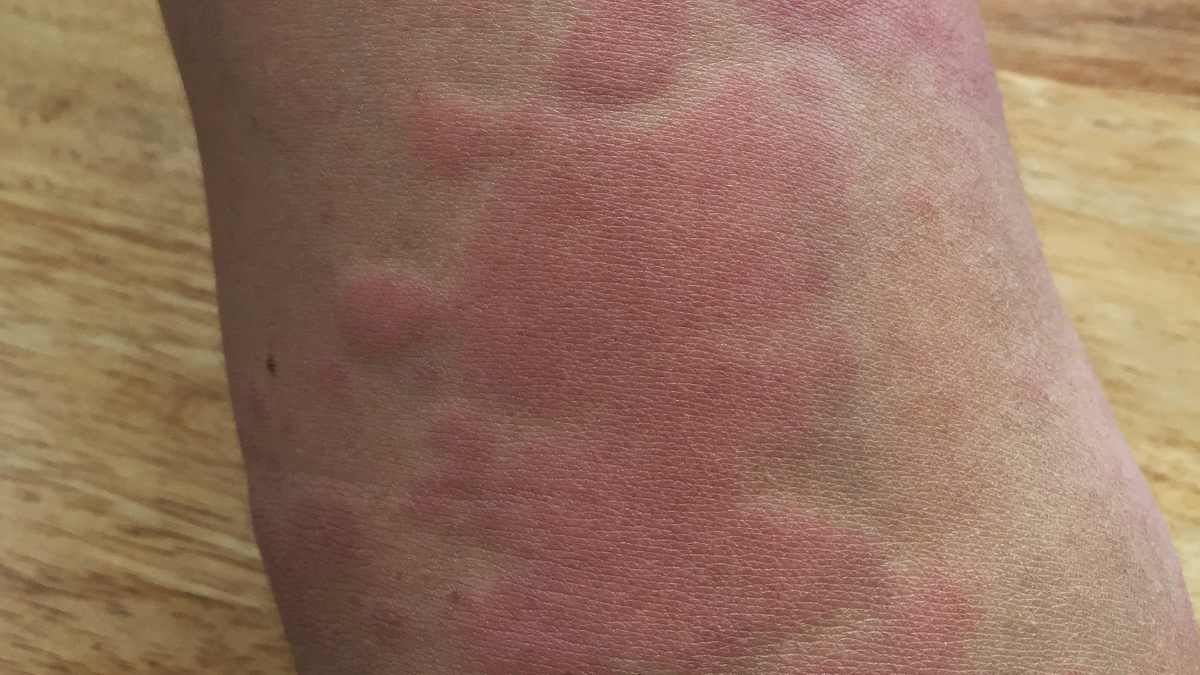
The visual characteristics of septic rash can vary widely, but certain common features can help in its identification. Typically, septic rash may present as red, inflamed patches on the skin, often accompanied by swelling and tenderness. The rash can appear suddenly and may spread rapidly, indicating a severe underlying infection.
In some cases, the rash may develop into blisters or pustules filled with fluid or pus, signifying a more severe infection. These lesions can rupture, leading to crusting or oozing, which may further complicate the clinical picture. The presence of these features often correlates with the severity of the infection and the patient’s overall condition.
The distribution of the rash can also provide valuable diagnostic clues. Septic rash may be localized to specific areas, such as around a wound or surgical site, or it may be more generalized, affecting larger areas of the body. This distribution can help healthcare providers determine the source of the infection and guide further diagnostic testing.
In addition to the rash itself, accompanying systemic symptoms such as fever, chills, and fatigue can further indicate the severity of the condition. The combination of these visual characteristics and systemic signs is critical for the accurate assessment of septic rash.
Differential Diagnosis: Distinguishing Septic Rash Types
Differentiating septic rash from other dermatological conditions is essential for appropriate management. Conditions such as cellulitis, impetigo, and drug eruptions can present with similar visual characteristics, making accurate diagnosis challenging. Cellulitis, for instance, is a bacterial skin infection that can cause redness and swelling but may not always be associated with systemic symptoms.
Impetigo, a highly contagious bacterial skin infection, typically presents as honey-colored crusted lesions and is more common in children. Unlike septic rash, impetigo is often localized and does not usually indicate a systemic infection. Understanding these distinctions is crucial for healthcare providers to avoid misdiagnosis and ensure effective treatment.
Drug eruptions can also mimic septic rash, presenting as widespread rashes accompanied by fever and malaise. However, these rashes often have a different distribution and may resolve upon discontinuation of the offending medication. A thorough patient history, including recent medication use, is vital for differentiating these conditions.
Other conditions, such as viral exanthems or autoimmune disorders, can also present with rashes that may be mistaken for septic rash. A comprehensive clinical evaluation, including patient history and physical examination, is essential for distinguishing between these various conditions.
Diagnostic Approaches for Septic Rash Evaluation
Evaluating septic rash requires a multi-faceted diagnostic approach. A thorough patient history is the first step, focusing on the onset of symptoms, recent infections, and any potential exposure to pathogens. This information can provide valuable insights into the possible cause of the rash and guide further testing.
Physical examination is crucial for assessing the rash’s characteristics, including its distribution, appearance, and associated symptoms. Healthcare providers often look for systemic signs of infection, such as fever, tachycardia, or hypotension, which can indicate the severity of the condition.
Laboratory tests play a significant role in diagnosing septic rash. Blood cultures are commonly performed to identify the causative organism, while complete blood counts can reveal signs of infection, such as elevated white blood cell counts. Additional tests, such as imaging studies, may be necessary if an underlying source of infection is suspected.
In some cases, a skin biopsy may be warranted to obtain a definitive diagnosis. This procedure can help differentiate septic rash from other dermatological conditions and guide appropriate treatment. Collaboration among healthcare providers, including dermatologists and infectious disease specialists, may be necessary for complex cases.
Treatment Options and Management Strategies for Septic Rash
The management of septic rash focuses primarily on treating the underlying infection. Antibiotic therapy is often the first line of treatment, with the choice of antibiotic guided by the identified pathogen and its susceptibility profile. In cases of severe infection or sepsis, intravenous antibiotics may be required for effective management.
Supportive care is also crucial in the treatment of septic rash. This may include fluid resuscitation, pain management, and monitoring for signs of systemic complications. In cases where the rash is associated with significant inflammation or discomfort, topical treatments may be employed to alleviate symptoms.
In addition to pharmacological interventions, addressing any underlying risk factors is essential for effective management. This may involve optimizing the patient’s overall health, managing chronic conditions, and implementing preventive measures to reduce the risk of future infections.
Follow-up care is critical to ensure that the infection is resolving and to monitor for any potential complications. Regular assessment of the rash and systemic symptoms can help guide ongoing treatment and support the patient’s recovery.
Conclusions:
Septic rash is a significant clinical indicator of underlying infections that require prompt recognition and treatment. Understanding its characteristics, causes, and management strategies is essential for healthcare providers and patients alike. Early intervention can greatly improve outcomes and reduce the risk of complications associated with septic conditions.
Read more
- Mayo Clinic – Sepsis – Comprehensive information on sepsis, including symptoms and treatment options.
- Centers for Disease Control and Prevention – Sepsis – An overview of sepsis, its causes, and prevention strategies.
- National Institutes of Health – Septic Rash – A detailed examination of septic rash and its clinical implications.
- American Academy of Dermatology – Skin Infections – Resources on various skin infections, including septic rash.
- WebMD – Understanding Skin Rashes – A guide to understanding different types of skin rashes and their causes.