Introduction:
Septic rash is a term that refers to a skin condition that arises as a result of systemic infections, particularly those that lead to sepsis. It is characterized by a variety of skin changes that can range from mild to severe, depending on the underlying cause and the individual’s health status. Understanding septic rash is crucial for timely diagnosis and treatment, as it can be a sign of a more serious condition that requires immediate medical attention. This article aims to provide a comprehensive overview of septic rash, including its causes, symptoms, diagnostic methods, treatment options, and prevention strategies.
Understanding Septic Rash: Definition and Overview
Septic rash can be defined as a skin manifestation that occurs due to an underlying infection that has systemic implications, often leading to sepsis. Sepsis is a life-threatening condition that arises when the body’s response to infection causes widespread inflammation. The skin changes associated with septic rash can include redness, swelling, and the presence of pustules or blisters. These changes are often indicative of the body’s immune response to infection and can serve as an important diagnostic marker.
The appearance of septic rash can vary significantly among individuals, depending on factors such as age, overall health, and the specific pathogen involved. In some cases, the rash may be localized, while in others, it may cover large areas of the body. The severity of the rash can also fluctuate, with some patients experiencing mild symptoms and others developing severe manifestations that require urgent medical intervention.
Recognizing septic rash is critical, as it can be one of the first signs of a serious underlying infection. Healthcare providers must be vigilant in assessing patients who present with skin changes, especially in those with risk factors for sepsis. Early identification and treatment of septic rash can lead to better outcomes and reduce the risk of complications associated with sepsis.
In summary, septic rash is a complex skin condition that serves as a potential indicator of systemic infection. Understanding its definition and overview is the first step in addressing the underlying causes and implementing appropriate management strategies.
Common Causes and Risk Factors of Septic Rash
The development of septic rash is often linked to various infectious agents, including bacteria, viruses, and fungi. Bacterial infections, particularly those caused by Staphylococcus aureus and Streptococcus pyogenes, are among the most common culprits. These pathogens can enter the body through cuts, abrasions, or other breaches in the skin, leading to localized infections that may progress to systemic involvement and sepsis.
In addition to bacterial infections, viral infections such as herpes simplex virus and varicella-zoster virus can also lead to septic rash. Fungal infections, particularly in immunocompromised individuals, may result in similar skin manifestations. Understanding the specific infectious agents involved is essential for guiding treatment and management strategies.
Certain risk factors can increase an individual’s likelihood of developing septic rash. These include underlying health conditions such as diabetes, chronic kidney disease, and immunosuppression due to medications or diseases. Additionally, age plays a role, with older adults being more susceptible to infections that can lead to septic rash. Hospitalization, particularly in intensive care settings, also elevates the risk due to increased exposure to pathogens.
Overall, recognizing the common causes and risk factors associated with septic rash is crucial for healthcare providers in identifying at-risk individuals and implementing preventive measures to reduce the incidence of this condition.
Clinical Presentation: Symptoms of Septic Rash
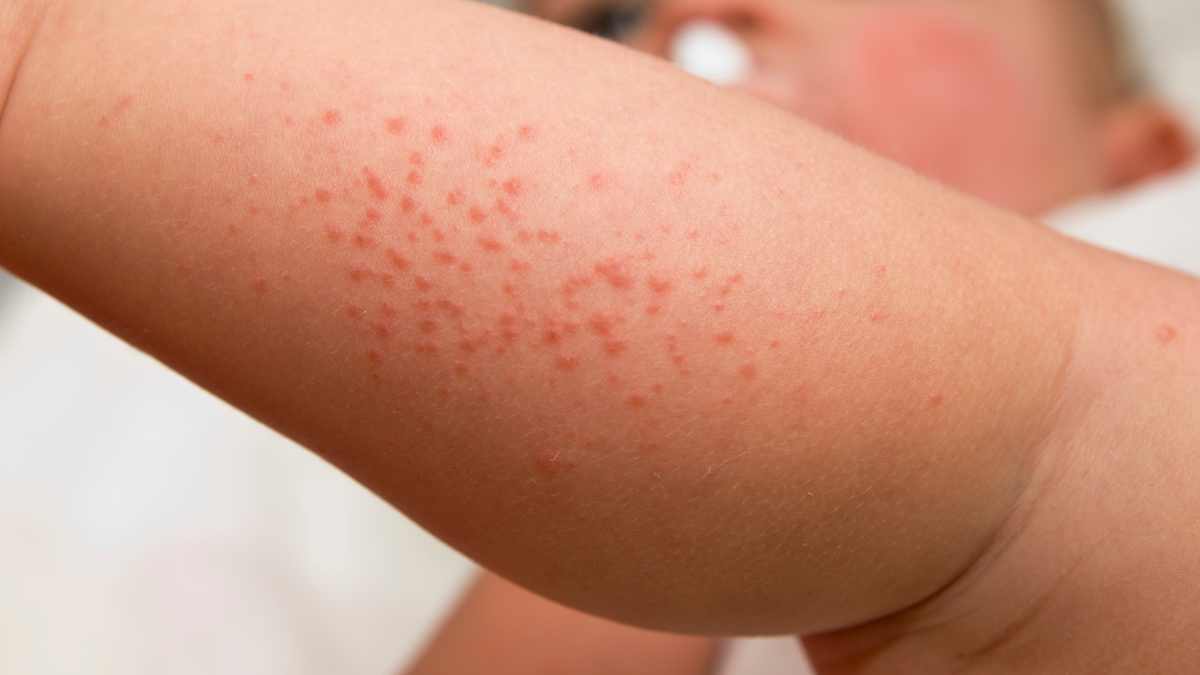
The clinical presentation of septic rash can vary widely, but it is typically characterized by several key symptoms. Patients may present with diffuse redness of the skin, often accompanied by warmth and swelling. This erythema may be localized or generalized, depending on the extent of the underlying infection. The presence of pustules, vesicles, or blisters may also be noted, indicating a more severe reaction to the infection.
In addition to skin changes, systemic symptoms may accompany septic rash. Patients often experience fever, chills, and malaise, which are indicative of the body’s inflammatory response to infection. Tachycardia and hypotension may also occur, particularly in cases where sepsis is present. It is essential to assess these systemic symptoms in conjunction with the skin manifestations to determine the severity of the condition.
The progression of septic rash can vary, with some individuals experiencing rapid deterioration of their skin condition and overall health. In severe cases, necrosis of the skin may occur, leading to complications such as cellulitis or even septic shock. Prompt recognition of these symptoms is vital for initiating appropriate treatment and preventing further complications.
In summary, the clinical presentation of septic rash includes a combination of localized skin changes and systemic symptoms. Understanding these manifestations is critical for healthcare providers in making timely and accurate diagnoses.
Diagnostic Approaches for Identifying Septic Rash
Diagnosing septic rash involves a comprehensive assessment that includes a detailed medical history, physical examination, and laboratory testing. The healthcare provider will begin by evaluating the patient’s symptoms, including the onset and duration of the rash, associated systemic symptoms, and any recent infections or hospitalizations. A thorough physical examination will help identify the characteristics of the rash and any signs of systemic involvement.
Laboratory tests play a crucial role in confirming the diagnosis of septic rash. Blood cultures are often performed to identify the specific pathogen responsible for the infection. Additionally, complete blood counts (CBC) may reveal elevated white blood cell counts, indicating an ongoing infection. Other tests, such as inflammatory markers (e.g., C-reactive protein), can provide further insight into the severity of the inflammatory response.
Imaging studies may also be utilized in certain cases, particularly if there is suspicion of deep tissue involvement or abscess formation. Ultrasound or CT scans can help visualize the extent of the infection and guide treatment decisions. It is essential for healthcare providers to utilize a combination of clinical assessment and diagnostic testing to accurately identify septic rash and its underlying causes.
In conclusion, a thorough diagnostic approach is essential for identifying septic rash. By combining clinical evaluation with laboratory and imaging studies, healthcare providers can ensure timely and effective management of this condition.
Treatment Options: Managing Septic Rash Effectively
The management of septic rash primarily focuses on addressing the underlying infection and alleviating the symptoms associated with the rash. Antibiotic therapy is often the cornerstone of treatment, particularly in cases where bacterial infections are identified. The choice of antibiotics will depend on the specific pathogen involved and may require adjustment based on culture results.
In addition to antibiotics, supportive care is crucial for patients with septic rash. This may include intravenous fluids to maintain hydration and support blood pressure, especially in cases of sepsis. Pain management and wound care are also essential components of treatment, as they help improve patient comfort and promote healing.
For patients with severe skin manifestations, such as extensive necrosis or blistering, surgical intervention may be necessary. Debridement of necrotic tissue can help prevent further infection and facilitate the healing process. In some cases, skin grafting may be required to restore the integrity of the skin.
Overall, effective management of septic rash requires a multidisciplinary approach that includes infectious disease specialists, dermatologists, and critical care providers. By addressing both the infection and the skin manifestations, healthcare providers can optimize patient outcomes and reduce the risk of complications.
Prevention Strategies to Reduce Septic Rash Incidence
Preventing septic rash involves implementing strategies to reduce the risk of infections that can lead to sepsis. One of the most effective measures is maintaining good hygiene practices, including regular handwashing and proper wound care. Individuals should be educated on the importance of cleaning and covering cuts or abrasions to minimize the risk of bacterial entry.
Vaccination is another critical component of prevention. Vaccines against common pathogens, such as influenza and pneumococcus, can help reduce the incidence of infections that may lead to septic rash. Additionally, individuals with chronic health conditions should work closely with their healthcare providers to manage their conditions effectively, as this can help lower their risk of developing infections.
In healthcare settings, strict infection control measures should be enforced to protect vulnerable patients. This includes proper sterilization of medical equipment, adherence to hand hygiene protocols, and the use of personal protective equipment (PPE) when necessary. Training healthcare staff on recognizing early signs of infection can also contribute to timely intervention and prevention of septic rash.
In summary, prevention strategies for septic rash focus on reducing the risk of infections through good hygiene practices, vaccination, and strict infection control measures in healthcare settings. By implementing these strategies, healthcare providers can help minimize the incidence of septic rash and improve patient outcomes.
Conclusions:
Septic rash is a significant clinical manifestation of underlying infections that can lead to sepsis. Understanding its definition, causes, symptoms, diagnostic approaches, treatment options, and prevention strategies is essential for healthcare providers in managing this condition effectively. Timely recognition and intervention are crucial for improving patient outcomes and reducing the risk of complications associated with septic rash.
Read more:
- Mayo Clinic – Sepsis – Comprehensive overview of sepsis, its causes, and associated skin manifestations.
- Cleveland Clinic – Septic Shock – Detailed information on septic shock, including symptoms and treatment options.
- Centers for Disease Control and Prevention (CDC) – Sepsis – CDC resources on sepsis, prevention, and management strategies.
- American Academy of Dermatology – Skin Infections – Information on various skin infections and their presentations, including septic rash.
- National Institute of Health – Sepsis and Skin – Research article discussing the relationship between sepsis and skin manifestations.