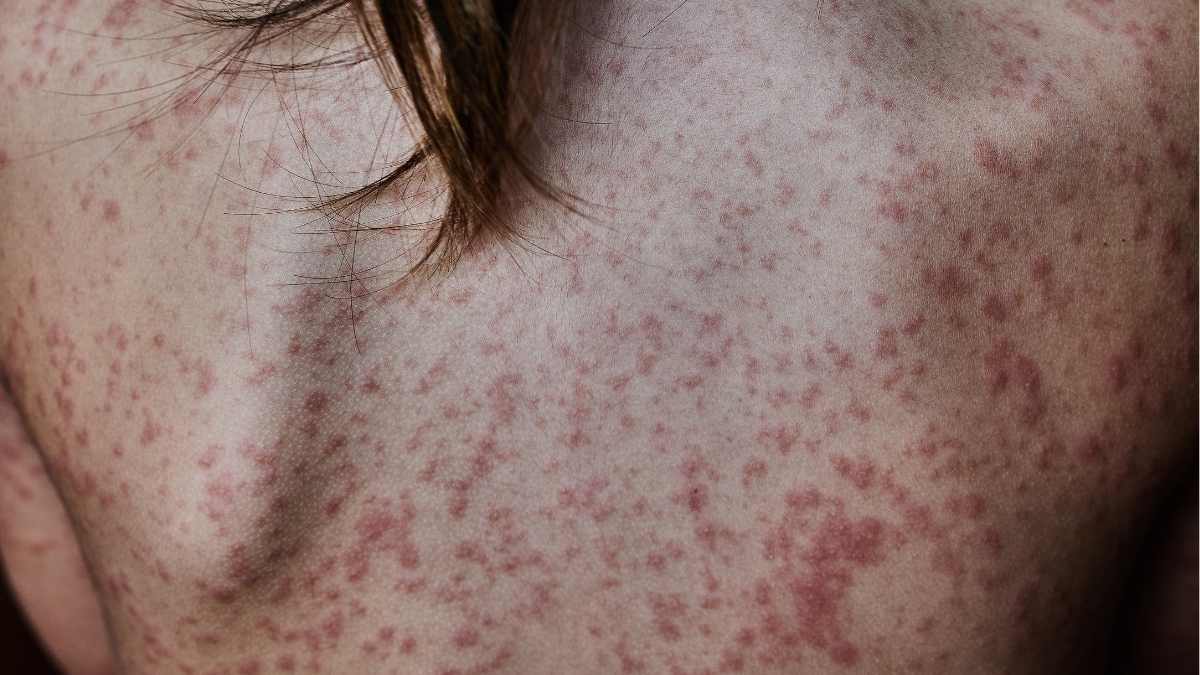
Introduction:
Rashes and itching are common dermatological issues that can significantly impact a person’s quality of life. Understanding the underlying causes and effective treatments is essential for managing these conditions. This article explores various options for relief, including over-the-counter medications, prescription treatments, and integrative approaches. By delving into the types of rashes, the role of antihistamines, topical corticosteroids, moisturizers, and when to seek medical advice, we aim to provide a comprehensive overview of the best strategies for managing rashes and itching.
Understanding Rashes: Types and Common Causes Explained
Rashes are characterized by changes in skin color, texture, or appearance, often accompanied by itching. They can arise from a multitude of causes, including allergic reactions, infections, autoimmune disorders, and irritants. Contact dermatitis, for instance, occurs when the skin comes into direct contact with an allergen or irritant, leading to localized inflammation and discomfort. Atopic dermatitis (eczema) is another prevalent type, often linked to genetic predisposition and environmental factors, resulting in chronic itching and skin lesions.
Infections can also lead to rashes. Fungal infections, such as ringworm, manifest as red, itchy patches, while viral infections, like chickenpox or herpes simplex, can produce widespread rashes accompanied by other systemic symptoms. Additionally, bacterial infections, such as impetigo, can cause crusty, itchy lesions that require prompt medical intervention. Understanding the specific type of rash is crucial for selecting the appropriate treatment.
Environmental factors, such as temperature and humidity, can exacerbate skin conditions. For example, excessive heat and sweating can lead to heat rash, characterized by small, itchy red bumps. Lifestyle factors, including stress and diet, may also play a role in skin health, triggering flare-ups in susceptible individuals. Identifying the cause of a rash is essential for effective management and prevention.
Finally, some rashes may indicate underlying systemic conditions, such as psoriasis or lupus. These chronic skin disorders require a comprehensive treatment approach that addresses both the skin symptoms and the underlying disease. Recognizing the type and cause of a rash is the first step toward effective treatment.
The Role of Antihistamines in Itch Relief and Management
Antihistamines are a cornerstone in the management of itching associated with allergic reactions and other dermatological conditions. These medications work by blocking the action of histamine, a chemical released during allergic responses that contributes to itching and inflammation. First-generation antihistamines, such as diphenhydramine (Benadryl), are effective but may cause sedation, making them suitable for nighttime use.
Second-generation antihistamines, like loratadine (Claritin) and cetirizine (Zyrtec), are less sedating and can be taken during the day without significant drowsiness. These medications are often preferred for chronic conditions, such as allergic rhinitis or chronic urticaria, where ongoing itch relief is necessary. They can help alleviate the discomfort associated with rashes while minimizing the risk of sedation.
In addition to their effectiveness in managing itching, antihistamines may also help reduce the severity of allergic reactions. For individuals with conditions like allergic contact dermatitis, taking antihistamines can provide symptomatic relief and improve overall quality of life. However, it is essential to consult with a healthcare provider to determine the most appropriate antihistamine based on individual symptoms and health history.
While antihistamines can be beneficial, they are not a cure-all. It is crucial to identify and address the underlying cause of the rash or itching to achieve long-term relief. In some cases, antihistamines may be used in conjunction with other treatments, such as topical corticosteroids, for a more comprehensive approach to management.
Topical Corticosteroids: Efficacy and Usage Guidelines
Topical corticosteroids are widely used to treat a variety of inflammatory skin conditions, including eczema, psoriasis, and allergic reactions. These medications work by reducing inflammation, redness, and itching, providing significant relief for affected individuals. Low-potency corticosteroids, such as hydrocortisone, are typically recommended for sensitive areas, while medium to high-potency corticosteroids are reserved for more severe cases or thicker skin areas.
When using topical corticosteroids, it is essential to follow specific guidelines to maximize efficacy and minimize potential side effects. Application should be limited to the affected areas, and the medication should be used sparingly to avoid skin thinning or other adverse effects. Intermittent use of corticosteroids can help manage flare-ups while reducing the risk of long-term complications.
Patients should also be aware of the importance of duration of use. Prolonged use of high-potency corticosteroids can lead to tolerance, where the skin becomes less responsive to treatment. To mitigate this, healthcare providers may recommend a rotation of different potencies or the incorporation of non-steroidal anti-inflammatory agents.
It is crucial to consult with a healthcare provider before starting topical corticosteroids, especially for children or individuals with pre-existing health conditions. A tailored treatment plan can ensure the right balance between effective symptom relief and the minimization of side effects.
Moisturizers and Emollients: A Key to Skin Barrier Repair
Moisturizers and emollients play a vital role in managing rashes and itching by restoring the skin barrier and preventing transepidermal water loss. Dry skin can exacerbate itching and inflammation, making it essential to maintain proper hydration. Regular application of moisturizers can help soothe irritated skin and provide a protective layer against environmental irritants.
There are various types of moisturizers available, including occlusives, humectants, and emollients. Occlusives, like petroleum jelly, create a barrier on the skin’s surface, preventing moisture loss. Humectants, such as glycerin and hyaluronic acid, attract water to the skin, while emollients smooth and soften the skin. A combination of these ingredients can provide optimal hydration and relief from itching.
For individuals with chronic skin conditions, such as eczema, incorporating a robust moisturizing routine can significantly improve skin health and reduce the frequency of flare-ups. It is advisable to apply moisturizers immediately after bathing to lock in moisture and enhance their effectiveness. Choosing fragrance-free and hypoallergenic products can further minimize the risk of irritation.
In addition to topical treatments, maintaining a healthy lifestyle, including proper hydration and a balanced diet, can support skin health. Individuals experiencing persistent rashes or itching should consult a dermatologist for personalized recommendations and treatment options.
When to Consider Prescription Medications for Severe Cases
In some instances, over-the-counter treatments may not provide adequate relief for rashes and itching. When symptoms are severe, persistent, or accompanied by other concerning signs, it may be time to consider prescription medications. Topical calcineurin inhibitors, such as tacrolimus and pimecrolimus, are often prescribed for conditions like eczema, especially in sensitive areas where corticosteroids may not be suitable for long-term use.
For more severe inflammatory conditions, systemic treatments may be necessary. Oral corticosteroids can provide rapid relief for acute flare-ups, while immunosuppressants, such as methotrexate or cyclosporine, may be indicated for chronic conditions that do not respond to conventional therapies. These medications require careful monitoring due to potential side effects, making it crucial to work closely with a healthcare provider.
In cases of allergic reactions, epinephrine auto-injectors may be prescribed for individuals at risk of anaphylaxis. This emergency medication can quickly reverse severe allergic reactions, including those that may present with widespread rashes and itching. Education on proper usage and recognition of symptoms is essential for individuals carrying these devices.
Ultimately, the decision to pursue prescription medications should be based on a thorough evaluation by a healthcare provider. A comprehensive approach that considers the patient’s medical history, lifestyle, and specific symptoms will ensure the most effective treatment plan.
Integrative Approaches: Complementary Therapies for Relief
In addition to conventional treatments, many individuals seek integrative approaches to manage rashes and itching. Complementary therapies, such as acupuncture, herbal remedies, and dietary modifications, can provide additional relief and support overall skin health. Acupuncture has been reported to help alleviate itching and inflammation by promoting circulation and balancing the body’s energy.
Herbal remedies, such as aloe vera, calendula, and chamomile, have been traditionally used for their soothing properties. These natural ingredients can be found in topical formulations or used in home remedies. However, it is crucial to approach herbal treatments with caution, as some individuals may experience allergic reactions or interactions with other medications.
Dietary changes can also play a role in managing skin conditions. Incorporating anti-inflammatory foods, such as omega-3 fatty acids found in fish and flaxseeds, may help reduce systemic inflammation and improve skin health. Conversely, some individuals may find that certain foods, like dairy or gluten, exacerbate their symptoms, warranting a personalized dietary approach.
While integrative therapies can complement conventional treatments, they should not replace medical advice or prescribed medications. It is essential to consult with a healthcare provider before embarking on any new treatment regimen, particularly for individuals with chronic skin conditions.
Conclusions:
Managing rashes and itching requires a multifaceted approach that considers the type of rash, underlying causes, and individual patient needs. From antihistamines and topical corticosteroids to moisturizers and integrative therapies, a variety of options are available for relief. It is essential to work closely with healthcare providers to develop a personalized treatment plan that addresses symptoms effectively while minimizing potential side effects. By understanding the various treatment modalities and their roles, individuals can take proactive steps toward achieving healthier skin and improved quality of life.
Read more
- American Academy of Dermatology – Itching and Rashes – A comprehensive resource on various skin conditions, including causes and treatments for itching and rashes.
- Mayo Clinic – Eczema – Detailed information on eczema, including symptoms, causes, and treatment options.
- Cleveland Clinic – Allergic Skin Reactions – An overview of allergic skin reactions, including rashes, their causes, and management strategies.
- National Eczema Association – Treatment Options – A resource dedicated to eczema treatment options, including both conventional and alternative therapies.
- WebMD – Antihistamines – An informative article discussing the role of antihistamines in treating allergies and associated symptoms.