Se hai un abbonamento attivo ACCEDI QUI
Introduction:
Itchy rashes can be a source of significant discomfort and distress for many individuals. Understanding the underlying mechanisms, common types, and treatment options available is crucial for effectively managing these conditions. This article delves into the complex interactions that lead to itchiness, explores various types of rashes known for their pruritic nature, and discusses how allergens contribute to skin irritations. Furthermore, we will examine diagnostic approaches, treatment options, and preventative strategies to help mitigate the discomfort associated with itchy rashes.
Understanding the Mechanisms Behind Itchy Rashes
Itching, or pruritus, is a complex sensation that often accompanies various skin conditions, particularly rashes. The sensation arises from the activation of specific nerve fibers in the skin, which transmit signals to the brain. These signals can be triggered by a variety of factors, including inflammation, irritation, and the release of certain chemicals such as histamines. Understanding these mechanisms is essential for developing effective treatments.
The skin serves as a barrier against external irritants and pathogens. When this barrier is compromised, whether through injury, infection, or an allergic reaction, inflammatory mediators are released. These substances can stimulate nerve endings, leading to the sensation of itch. The interplay between the immune system and the nervous system is crucial in the development of itchy rashes. Conditions like eczema and psoriasis exemplify how chronic inflammation can lead to persistent itching.
Moreover, psychological factors can also play a role in the perception of itch. Stress and anxiety can exacerbate the sensation, creating a feedback loop where itching leads to more stress, which in turn increases the urge to scratch. This highlights the importance of a holistic approach in managing itchy rashes.
Finally, certain systemic conditions, such as liver disease or kidney dysfunction, can lead to generalized itching without a visible rash. Understanding these underlying mechanisms is vital for clinicians to provide appropriate care and guidance to patients experiencing itchy skin conditions.
Common Types of Rashes That Cause Intense Itching
Several types of rashes are particularly notorious for causing intense itching. One of the most common is atopic dermatitis, often seen in children but can persist into adulthood. This chronic condition is characterized by dry, inflamed skin that can become extremely itchy, especially during flare-ups. The itch-scratch cycle can exacerbate the condition, leading to further skin damage and increased discomfort.
Another prevalent rash associated with itching is contact dermatitis, which occurs when the skin comes into direct contact with an irritant or allergen. Common triggers include poison ivy, certain metals, and fragrances. The resulting rash can be red, swollen, and intensely itchy, often requiring avoidance of the offending substance for resolution. Identifying the specific allergen is critical for effective management.
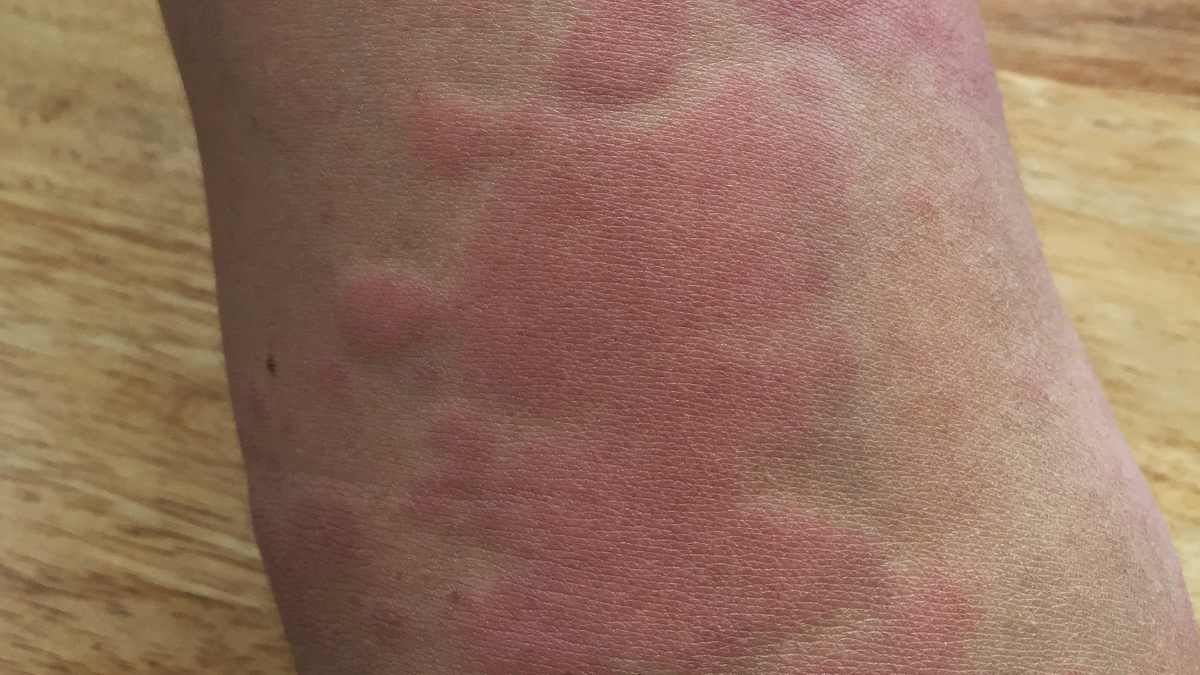
Urticaria, or hives, is another type of rash that can cause severe itching. It appears as raised, red welts on the skin and can result from various triggers, including food, medications, or environmental factors. The rapid onset and resolution of hives can be distressing, making prompt treatment essential.
Lastly, conditions like scabies and lice infestations lead to intense itching due to the presence of parasites. These conditions require specific treatments to eliminate the underlying cause and alleviate symptoms. Recognizing the type of rash is crucial in determining the appropriate course of action.
The Role of Allergens in Itchy Skin Conditions
Allergens play a significant role in the development of itchy skin conditions. When the immune system mistakenly identifies a harmless substance as a threat, it triggers an allergic reaction. This response can lead to the release of histamines and other inflammatory mediators, resulting in itching and rash formation. Common allergens include pollen, pet dander, and certain foods.
In cases of allergic contact dermatitis, the skin reacts to specific substances it has come into contact with, leading to localized itching and inflammation. Identifying and avoiding these allergens is critical for preventing future outbreaks. Patch testing is often employed by dermatologists to determine the specific allergens responsible for an individual’s symptoms.
Additionally, systemic allergies can also contribute to itching. Conditions such as allergic rhinitis or food allergies may manifest with skin symptoms, including rashes and intense itching. This systemic response underscores the interconnectedness of the immune system and skin health.
Understanding the role of allergens is essential for both patients and healthcare providers. By recognizing potential triggers and implementing avoidance strategies, individuals can significantly reduce the incidence and severity of itchy rashes.
Diagnosing Itchy Rashes: Clinical Approaches and Tools
Diagnosing itchy rashes involves a comprehensive clinical evaluation. Healthcare providers typically begin with a thorough medical history, including any known allergies, recent exposures, and the duration and characteristics of the rash. A detailed history can provide valuable clues for diagnosis.
Physical examination plays a crucial role in identifying the type of rash. Providers assess the appearance, distribution, and associated symptoms to differentiate between various conditions. For instance, the presence of vesicles may suggest herpes simplex virus infection, while scaling may indicate psoriasis.
In some cases, additional diagnostic tools may be necessary. Skin scrapings, biopsies, or cultures can help identify infectious agents or rule out other conditions. Allergy testing, including skin prick tests or blood tests, can also be beneficial in determining specific allergens.
Ultimately, an accurate diagnosis is essential for effective management. By employing a combination of clinical evaluation and diagnostic tools, healthcare providers can tailor treatment strategies to address the underlying cause of the itchy rash.
Treatment Options for Managing Itchy Skin Rashes
Effective management of itchy skin rashes often requires a multifaceted approach. Topical treatments, such as corticosteroids, are commonly prescribed to reduce inflammation and alleviate itching. These medications can be applied directly to the affected area and are often effective for conditions like eczema and contact dermatitis.
In cases of more severe itching, systemic treatments may be necessary. Antihistamines are frequently used to counteract the effects of histamines released during allergic reactions. These medications can help alleviate itching and improve overall comfort. In some instances, immunosuppressive agents may be prescribed for chronic conditions that do not respond to standard treatments.
For infections caused by parasites, such as scabies or lice, specific antiparasitic medications are required. These treatments target the underlying cause of the itching and are essential for resolution.
Additionally, non-pharmacological approaches, such as moisturizing the skin and avoiding known irritants, can play a significant role in managing symptoms. Education on proper skincare and lifestyle modifications is crucial for long-term management.
Preventative Strategies to Reduce Rash-Related Itching
Preventing itchy rashes involves a combination of lifestyle modifications and proactive measures. One of the most effective strategies is to identify and avoid known allergens and irritants. This may include using hypoallergenic products, wearing protective clothing, and avoiding certain foods.
Maintaining proper skin hydration is also essential. Regularly applying moisturizers can help strengthen the skin barrier, reducing the likelihood of dryness and irritation. This is particularly important for individuals with conditions like eczema, where the skin barrier is often compromised.
Practicing good hygiene and avoiding excessive heat and sweating can also help prevent flare-ups. In environments where allergens are prevalent, such as during pollen season, staying indoors and using air purifiers can minimize exposure.
Lastly, managing stress through relaxation techniques or therapy can help reduce the severity of itching. Since psychological factors can exacerbate itch, addressing these can lead to improved outcomes. By implementing these preventative strategies, individuals can significantly reduce the incidence and severity of itchy rashes.
Conclusions:
Itchy rashes can significantly impact an individual’s quality of life, but understanding the underlying mechanisms, common types, and treatment options available can help manage symptoms effectively. By recognizing the role of allergens, employing appropriate diagnostic tools, and utilizing both pharmacological and non-pharmacological treatments, individuals can find relief from itching. Preventative strategies also play a crucial role in minimizing future occurrences. With the right approach, it is possible to manage and reduce the discomfort associated with itchy rashes.
Read more
- American Academy of Dermatology – Itchy Skin – Comprehensive information on causes and treatments for itchy skin.
- Mayo Clinic – Eczema – Detailed overview of eczema, a common cause of itchy rashes, including symptoms and management.
- National Eczema Association – Itch – Resources and strategies for managing itch associated with eczema.
- Cleveland Clinic – Contact Dermatitis – Information on contact dermatitis, its causes, and treatment options.
- WebMD – Hives (Urticaria) – Overview of hives, including symptoms, causes, and treatment strategies.